| Last updated: Friday, January 28, 2005 |
About surgery for traumatic instabilityHere is some patient information typically given to a patient before a repair for traumatic instability. However, this will vary with the surgeon, the patient and the repair. If you have are going to have such a repair, only your surgeon can give you specific information relative to your procedure. Traumatic instability When a major force is applied to the arm, the supporting ligaments of the shoulder joint may be torn. Sometimes these ligaments heal spontaneously in the proper location so that the stability of the shoulder is regained. On other occasions, strong healing to the appropriate location does not occur, leaving the shoulder unstable when it is put in certain specific positions. We refer to this as traumatic instability of the shoulder. These injuries most commonly arise from situations in which the elevated arm is forced violently backward such as in a fall while skiing. If this is the situation, one may elect to avoid the positions in which the shoulder feels unstable, recognizing that this may require giving up certain activities. Alternatively, one may seek a surgical repair of the torn structures with a goal to regain some of the functional abilities that were lost. Who should consider this surgery We consider surgical treatment for informed patients who are unwilling to accept the functional limitations imposed by recurrent traumatic instability.Goals of surgery The ligaments are almost always torn from the front bottom part of the socket of the shoulder. We can often repair this injury by sewing the ligaments back to the bone from which they were torn. We make an incision in the lower front skin creases of the shoulder and gain access to the joint between two of its major muscles: the deltoid and the pectoralis major. The ligaments are reattached by roughening up the edge of the bony socket and placing small drill holes in the lip of this socket. Sutures are passed through these drill holes and through the ligaments so that when the sutures are tied the ligaments are held in the appropriate place for healing.Risks of surgery The risks of this surgery include, but are not limited, to:
Post-surgery limitations For three to four weeks after the surgery one must protect the shoulder from elevation above the horizontal and from rotation away from the body. It is important to carry out isometric strengthening exercises which are done with the arm in a sling. After this first period of protection, gentle range of motion and additional strengthening exercises are added. During the second six weeks we emphasize shoulder range of motion, strength, endurance, and coordination. Usually patients can resume rigorous physical activities three months after the operation provided they have regained excellent strength, coordination, endurance, and a near-normal range of motion of the shoulder. |
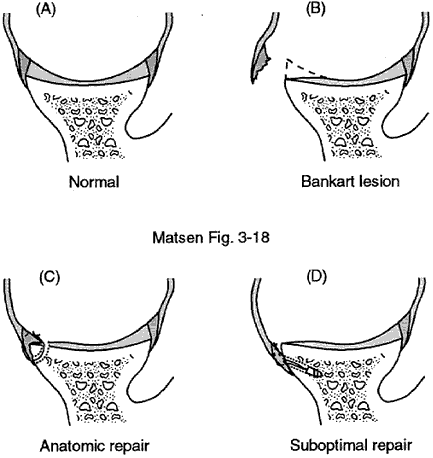
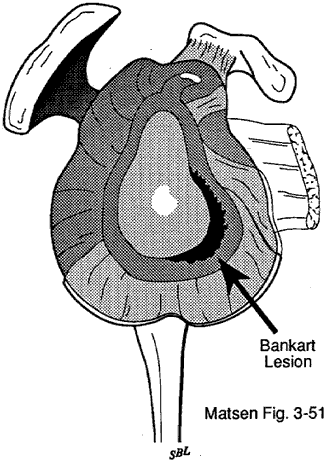
Details of the surgeryAbout the surgery Here are some details regarding surgery for the management of traumatic anterior glenohumeral instability. This section on surgical treatment concerns the management only of patients who have traumatic anterior inferior glenohumeral instability that has been established preoperatively by careful history and physical examination. The indications for surgical treatment of this lesion are persistent significant functional deficits (apprehension, subluxation, dislocation) in abduction, external rotation, and extension resulting from an initial episode which was sufficiently traumatic to tear part of the major capsuloligamentous supporting structures of the glenohumeral joint. For patients not meeting these strict criteria, we use the methods of treatment for atraumatic instability. The goals of treating traumatic anterior inferior glenohumeral instability are to repair the traumatic lesion safely, restoring the attachment of the glenohumeral ligaments, capsule, and labrum to the rim of the glenoid. By assuring that reattachment occurs to the rim, the effective depth of the glenoid is restored. By definition these patients do not have a functional problem with capsular laxity, thus, capsular reefing is not a part of this procedure. Surgical technique The goal of the surgical treatment for traumatic anterior glenohumeral instability is the safe and secure reattachment of the detached glenohumeral ligaments to the lip of the glenoid from which they were avulsed. No attempt is made to modify the normal laxity of the anterior capsule. This anatomic reattachment should reestablish not only the capsuloligamentous check rein but also the fossa-deepening effect of the glenoid labrum. A repair that is secure from the time of surgery is highly desirable in that it allows patients to resume many of their activities of daily living while the repair is healing. A repair that is secure from the time of surgery also allows controlled mobilization, thereby minimizing the possibility of unwanted stiffness. In traumatic anterior instability, the absence of the normal anterior glenoid lip can often be demonstrated by the lack of resistance to anterior glenohumeral translation on the sheer test. The patient is positioned in a 30 degree inclined beach chair position with the arm free over the edge of the table. No sand bag is used underneath the shoulder blade. Prepping and draping allow the arm to be freely moveable and allows generous exposure to the anterior aspect of the shoulder. The skin incision is marked in the dominant anterior axillary crease which is revealed when the arm is adducted. After the incision is marked, an adhesive drape is applied and the incision is made. The deltopectoral groove is entered, retracting the cephalic vein laterally with the deltoid. The clavipectoral fossa is incised just lateral to the short head of the biceps, up to but not through the coracoacromial ligament. We routinely palpate the axillary nerve as it crosses the anteroinferior border of the subscapularis. A Balfour retractor is useful in the exposure. The anterior humeral circumflex vessels can usually be protected by bluntly dissecting them off of the subscapularis muscle at its inferior border. The subscapularis tendon and the subjacent capsule are incised 5 mm medial to their insertion at the lesser tuberosity. This incision starts superiorly at the upper rolled edge of the subscapularis and extends inferiorly to the bottom of the lesser tuberosity. It is important that the incision through the subscapularis tendon leaves strong tendinous material on both sides of the incision to facilitate a secure repair at the conclusion of the procedure. We examine the joint for loose bodies, for displaced fragments of glenoid labrum and particularly in older patients for evidence of rotator cuff tears. We can usually palpate a posterior lateral humeral head defect. The capsule and subscapularis are then retracted medially as a unit and a humeral head retractor is placed in the joint. An angled retractor is used to expose the glenoid lip and to identify the capsuloligamentous avulsion know as the Bankart defect. Occasionally flimsy attempts to heal the lesion will temporarily obliterate the defect. However, in these cases a blunt elevator will easily reveal the typical lesion in the anterior-inferior quadrant of the glenoid. A spiked retractor is then placed through the ligamentous avulsion to expose the defect at the glenoid lip. |
|
|||||||||||||||||
| We roughen the anterior, non-articular aspect of the glenoid lip with a curette or a motorized burr, taking care not to compromise the bony strength of the glenoid lip. We mark the intended sites for holes in the glenoid lip with cautery. A i.7 mm drill is then used to make holes on the articular aspect of the glenoid 3 to 4 mm back from the edge of the lip to ensure a sufficiently strong bony bridge. We place these holes 5 to 6 mm apart; thus the size of the defect dictates the number of holes used for reattachment of the avulsed capsule. Corresponding slots are placed on the anterior non-articular aspect of the glenoid. Using a 000 angled curette, we establish continuity between the corresponding slots and holes.
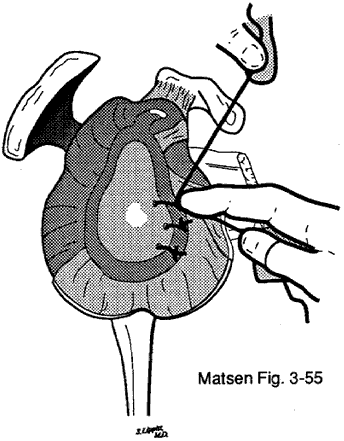
We then pass a strong number 2 absorbable braided suture through the holes in the glenoid lip using a trocar needle and an angled needle holder. After each suture is placed through the glenoid lip, the integrity of the bony bridge is checked by a firm pull on the suture. At this point in the procedure it is again useful to verify the location of the axillary nerve. The spiked retractor is then removed from the lesion and an angled retractor is used to expose the trailing medial edge of the avulsed capsule. Next, using the trocar needle, we pass the end of the suture, exiting the anterior non-articular aspect of the glenoid lip through the trailing medial edge of the capsule, taking care to include the glenoid labrum, if present. We avoid including any more capsule than necessary to obtain a firm purchase; this prevents unwanted tightening of the anteroinferior capsule. In larger glenohumeral ligament avulsions, the detached medial edge of the capsule tends to sag inferiorly; thus, in these larger lesions an effort needs to be made to pass the needle through the capsule slightly inferior to the bony holes in the glenoid. At the time of closure the inferiorly sagging medial capsule will be repositioned anatomically. Once the sutures have been passed through the capsule, they are tied so that the labrum and medial edge of the capsule are positioned on the glenoid lip. The knots are tied so that they come to rest over the capsule, rather than on the articular surface of the glenoid. Once these sutures are tied, the smooth continuity between the articular surface of the glenoid fossa and the capsule should be reestablished. No stepoff or discontinuity in the capsule should be present. If such a discontinuity is noted, the sutures are replaced so that they obliterate the defect. At the conclusion of the surgical repair the capsule and subscapularis tendon are repaired anatomically to their mates at the lesser tuberosity. The integrity of the axillary nerve, which has been monitored through the case, is again verified on closure. MoviesAfter the surgery The sheer test is checked again after the repair. The shoulder should have at least 30 degrees of external rotation at the side after the subscapularis/capsular repair. A standard wound closure is carried out, using a subcuticular suture, which is removed at three days. Within the first few days after surgery, reliable patients are encouraged to use the arm up to 90 degrees of elevation in the anterior plane and out to zero degrees of external rotation. This allows sufficient range of motion to perform most activities of daily living, such as eating and personal hygiene, as well as certain vocational activities, such as writing and typing. Gripping, isometric external rotation, and isometric abduction exercises are started immediately after surgery to minimize effects of disuse. If a patient does not appear able to comply with this restricted use program, we require that the arm be kept in a sling for three weeks. At three weeks the patient should return for an examination and should have at least 90 degrees of elevation and external rotation to zero degrees. From three weeks to six weeks postoperatively, the patient is instructed to increase the range of motion to 140 degrees of elevation and 40 degrees of external rotation. At six weeks after surgery, if there is good evidence of active control of the shoulder, gentle repetitive activities such as swimming and using a rowing machine may be instituted to help with coordination, strength, and endurance of the shoulder. More vigorous activities such as basketball, volleyball, throwing, and serving in tennis should not be started until three months and only then if there is excellent strength, endurance, range of motion, and coordination of the shoulder. Movies
|
||||||||||||||||||
RehabilitationAvoid stiffness Patients are usually able to conduct their own postoperative rehabilitation program with instructions from a physical therapist or a physician. Vigilance must be exercised for patients over 35 years of age to be sure that they do not develop unwanted postoperative stiffness. Thus, particularly for these patients, the three-week and six-week checks are very important to make sure that the ranges of elevation and external rotation are respectively 90 and 0 degrees at three weeks, and 140 and 40 degrees at six weeks. Instructions for rehabilitation These are typical instructions given to a patient after a repair for traumatic instability. However, the program will vary with the surgeon, the patient, and the repair. If you have had such a repair, only your surgeon can give you instructions on the postoperative management. Do not do any exercises after surgery except after consultation with your physician. After your surgical repair, your arm is in a sling to assure that it heals properly. If this sling is not comfortable, be sure to let your doctor know immediately. You may remove your arm from the sling to perform your exercises. These include lying down on your back and lifting your arm so that the elbow points straight up. In the second exercise, also performed lying on your back, you rotate your forearm away from your stomach until it points straight ahead. You need to start exercises in your sling right away. First you need to maintain the strength of your grip by squeezing a ball, sponge, or putty several hundred times a day. Second you should perform three minutes of gentle isometric exercises at least three times a day against some fixed object - pushing your wrist outward, pushing your hand forward, pushing your elbow outward, and pushing the elbow back. These exercises are designed to maintain your muscle tone. The shoulder is not moved during these exercises. They should be comfortable. You will return to the office three weeks after surgery. If everything is healing properly, you will begin weaning yourself from the sling at that time. At three weeks after surgery, you can increase your overhead reach until your arm is close to your ear and until your forearm can be externally rotated 40 degrees from the straight ahead position. You need to continue your previous isometric exercises and can add internal and external rotation strengthening using rubber tubing. You then progress by using your arm for light activities of daily living, avoiding the positions that used to be unstable. Always avoid "checking" your shoulder to see if it is stable. You must not lift over 10 pounds for the first six months after your surgery. After six weeks you can begin gentle, well-controlled, repetitive activities with your shoulder such as swimming or using a rowing machine, provided that these activities are comfortable for you. At three months it is often appropriate to implement the full home exercise program. You cannot return to contact sports or heavy work for at least three months after this surgery, and then only if you have excellent strength and coordinated control of your shoulder. If you have any questions at any time, please let your doctor know. |
ConclusionIn summary |