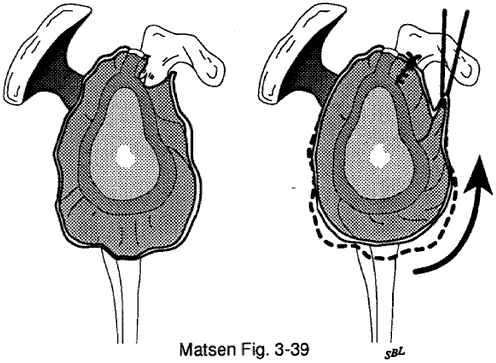
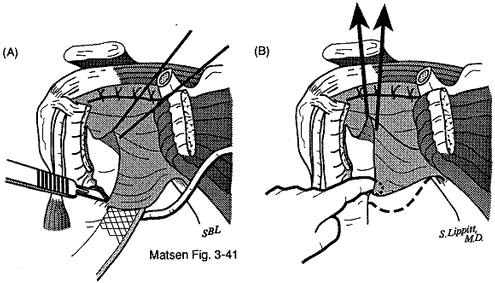
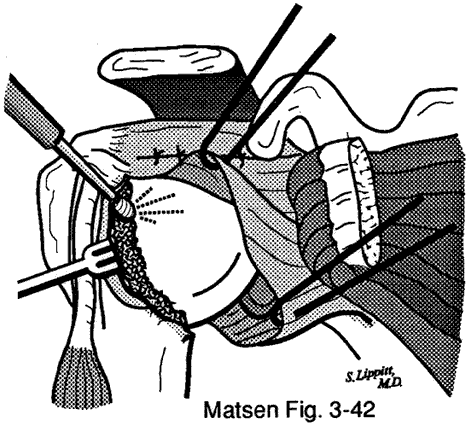
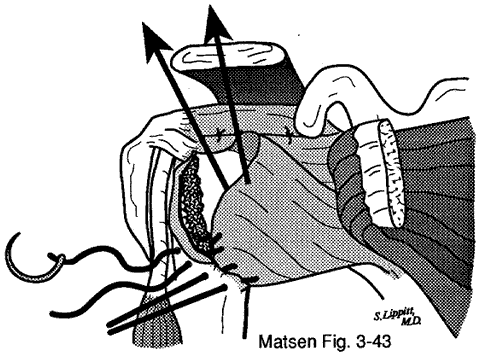
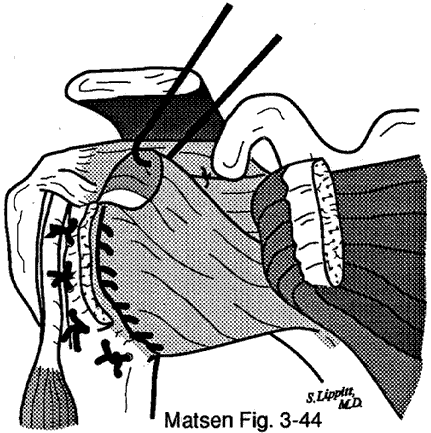
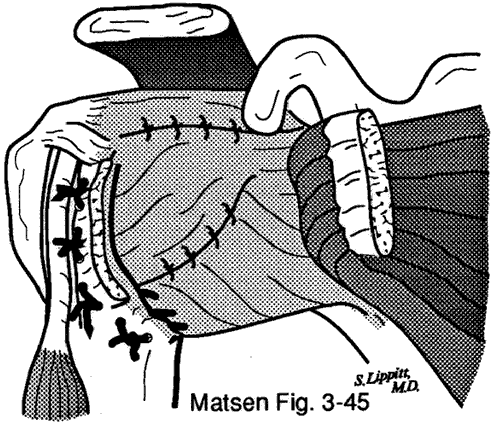
About surgery for atraumatic instabilityThis is the information which might be shared with patients as they consider surgical management of atraumatic instability. Before it can be applied to a specific clinical situation, however, it needs to be tailored to the patient, the problem, and the surgeon. Management of atraumatic instability A shoulder may have problems with instability even though there has not been a major traumatic injury. As a result, the shoulder may slip or feel unstable with certain activities. Most often, atraumatic shoulder instability can be managed by restoring the normal strength and coordinated use of the shoulder through a reconditioning program. Rarely, the instability is so severe that surgery is considered as an adjunct to the exercise and training program. Shoulder surgery itself cannot "fix" the problem of atraumatic instability because there is no simple rip to sew up. Instead, the goal of shoulder surgery for this type of instability is to tighten the tissues around the shoulder joint, restricting its range of motion but also helping add some stability. |
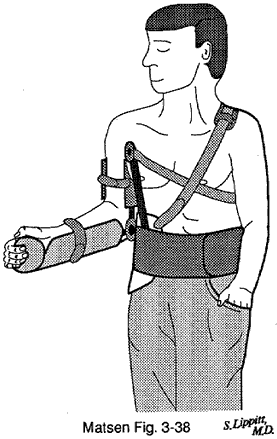
RehabilitationPostoperative rehab With the arm in the orthosis, the patient is started on grip strengthening, elbow range of motion, isometric external rotation, and isometric abduction shoulder exercises. The brace is usually continued for one month, although longer periods may be used for individuals who are extremely lax, and shorter periods may be used for individuals over 25 years of age who may be prone to excessive stiffness. The patient is then weaned from the orthosis over a period of a week. During this time the patient is taught to elevate the arm in the coronal plane only, to continue the cuff and deltoid strengthening, and to avoid any activities that may challenge the repair. From this point, range of motion is gained only with active exercises; no passive stretching is used. Lifting of more than 10 pounds is delayed for six months. Sports are delayed for at least one year after surgery and are permitted only if the patient has excellent strength and dynamic control of the shoulder. The patient needs to understand in detail the importance of this program. Rehabilitation instructions These are typical instructions given to a patient after a repair for atraumatic instability. However, the program will vary with the surgeon, the patient, and the repair. If you have had such a repair, only your surgeon can give you instructions on the postoperative management. Do not do any exercises after surgery except after consultation with your physician. The arm may be placed in a brace to assure that it heals properly. If this brace is not comfortable, be sure to let your doctor know immediately. For one month after the operation your arm must stay in the brace. If someone can hold your arm in the correct position for you during bathing, you may briefly remove it for this purpose. Otherwise, you should clean yourself twice a day using an alcohol sponge underneath the straps of the brace. You can put on a shirt if someone can help you by keeping your arm in the correct position while your arm is threaded through the sleeve. Otherwise you should wear loose-fitting clothes over the brace. Each day you can loosen the forearm straps to put your elbow through a range of motion. Your doctor may start exercises such as these while you are still in your brace. First, you need to maintain the strength of your grip by squeezing a ball, sponge, or putty several hundred times a day. Second, you should perform 3 minutes of gentle isometric exercises at least three times a day against some fixed object--pushing your wrist outward, pushing your hand forward, pushing your elbow outward, and pushing the elbow back. These exercises are designed to maintain your muscle tone. The shoulder is not moved during these exercises. The exercises should be comfortable. You should return to the office at one month after surgery. If everything is healing properly, you may begin weaning yourself from the brace at that time. In the weaning process you will start moving your shoulder out to the side, avoiding the positions that used to be symptomatic for you. You may find it reassuring to sleep in your brace for another week. You will regain your motion on your own, moving your shoulder under its own motor power and specifically avoiding any stretching. You need to continue your previous isometric exercises and can add progressively the same exercises you did before surgery. Always avoid "checking" your shoulder to see if it is stable. You must not lift more than 10 pounds for the first six months after your surgery. After four months you can begin gentle, well-controlled, repetitive activities with your shoulder, such as swimming or using a rowing machine, provided that these activities are comfortable for you. You cannot return to contact sports or heavy work for at least one year after this surgery, and then only if you have excellent strength and coordinated control of your shoulder. If you have any questions at any time, please let your doctor know. |