Edited by Nick Hernandez, M.D., Assistant Professor, UW Orthopaedics & Hip & Knee
What options are available for a patient who has severe arthritis (sometimes called "bone-on-bone") throughout the knee?
When the weight-bearing surface of a joint called cartilage is lost or severely damaged that condition is called arthritis or degenerative joint disease. Normal cartilage is very smooth and slippery. Arthritic cartilage is rough and cracked. When the cartilage is gone completely bones beneath the cartilage on opposite sides of the joint rub against one another and this can be quite painful.
Usually before considering surgery most knee specialists would recommend a course of non-operative management to see whether relief can be obtained without needing to go through the inconvenience and risk of surgery. Non-operative treatments for arthritis include pills (like Tylenol or an anti-inflammatory such as ibuprofen or Celebrex) or joint injections (such as cortisone-type shots ). Some kinds of non-operative management don't involve medications at all: weight loss if appropriate activity modifications and sometimes use of a cane or a brace can help. But for some people with severe arthritis these aren't enough and the pain continues despite these efforts. In those instances surgery may be reasonable.
For young people with arthritis (usually under age 40-50) it is desirable to avoid a joint replacement if possible since patients in that age group are very likely to outlive the joint replacement. In those individuals who represent a very unusual circumstance there are other surgical options available. It is reasonable to talk to your physician to find out which is best for you.
For people in "middle age" or older who have endstage arthritis and symptoms that are activity-limiting despite nonsurgical options, a knee replacement may be a reasonable choice to relieve the pain of knee arthritis and restore a reasonable level of function. There are two kinds of knee replacements: partial and total.
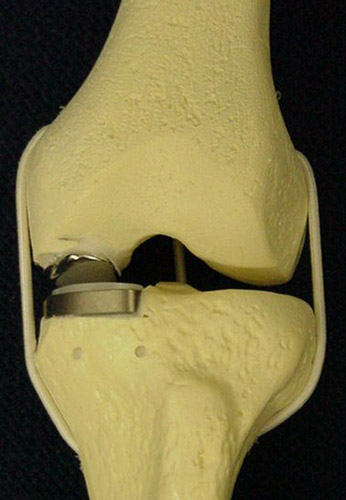
Model of a partial knee
replacement.
When the arthritis in the knee is confined to just one side and as long as the pain is only on one side of the knee as well sometimes a minimally-invasive partial knee replacement can be performed (see figure 1). For more detail about this procedure click here.
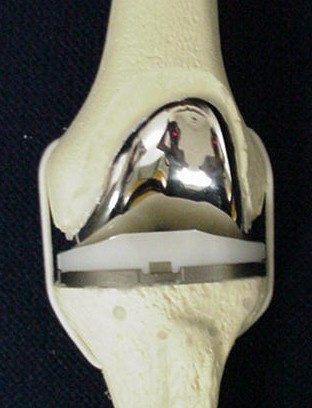
For people with arthritis throughout the knee (sometimes called bi- or tri-compartmental arthritis) a total knee replacement is still the most reliable operation we have. More than 90 percent of patients who undergo this operation will be very satisfied with it and they now last more than 10 years in more than 90 percent of patients. This procedure involves replacing the weight-bearing surfaces of the knee with metal and a high-performance plastic (see figure 2). Most patients are able to walk without pain once they recover from this procedure and many also resume their preferred (non-impact) recreational activities such as golf cross-country skiing dancing or riding a bicycle.
The best way to learn more about these procedures (or to find out whether it is a good option for you) is to speak with a joint replacement specialist or a good orthopedic surgeon who is comfortable with complex knee surgery.
Model of a traditional
total knee replacement.
The patella (knee cap)
is not shown in this model.
What surgery is available for a torn knee meniscus
While in the past, surgeons believed that arthroscopic surgery was a reasonable intervention for meniscus tears in adults who are middle aged or beyond, newer studies have called that belief into question. In general, for most patients with degenerative meniscus tears are better managed without surgery, whether with short courses of non-narcotic pills (Tylenol or anti-inflammatories), joint injections (like cortisone), or physical therapy.
The best way to decide what procedure (if any) is best for you is by seeing a surgeon with considerable experience in the surgical and non-surgical approaches that are available to treat knee problems of this type, but if a surgeon recommends arthroscopic surgery for a degenerative meniscus tear, it is reasonable to ask some direct questions about what evidence supports (and what evidence opposes) this recommendation. A great deal has been published on this in the last few years.
Replacing both knees at the same time.
This is an excellent question and like many good questions the answer is somewhat complicated. It is almost always technically possible to replace both knees at once. However, one has to ask: what would be gained or given up by doing this? Studies disagree. In general, my take on what we know is that the overall time to full recovery is shortened by doing knees at the same time but you take some increased risk to gain this advantage. Here's the summary as I interpret it:
The benefit of same-day both-knee surgery: The time to full recovery is shorter. If that does not seem intuitive think about it this way: If you figure it will take between 2-3 months to really start to feel right after a knee replacement and you do that twice that's 4-6 months of total recovery time. If you do them both the same day you go through the experience once and the whole thing is behind you in 2-3 months.
The disadvantage of same-day both-knee surgery: The surgical risk appears to be increased. The types of complications that were more common in patients having the knees done together included:
- temporary disorientation after surgery,
- the need for blood transfusions, and
- severe cardiac complications (which can be fatal).
If the complication rates were doubled in same-day both-knee surgery we'd call that a tie since you'd have to have the operation twice if you did it on separate surgical dates. However the complication rates for all the complications listed above are more than double with same-day both-knee surgery. In addition, the overall length of hospital stay may be a bit longer with same-day both-knee surgery.
So in view of this why would anyone want to do them both at once? My observation is there are two sets of feelings on the part of patients about this. Some people are risk-averse and want to minimize the risk as completely as possible; clearly they would want to do one knee at a time. Other people are what I call therapy-averse (or pain-averse) meaning they want to minimize the overall length of time they are either in physical therapy (perhaps for work reasons) and the overall length of time they are uncomfortable from the surgery. Provided they don't mind the increase in risk they may be good candidates for same-day both-knee surgery, though as a surgeon I am so risk averse that I seldom will recommend this.
And, of course, there are some people whose medical conditions (like a history of prior heart attacks) or very advanced age would make it simply a bad idea to do both at once.
It's obviously a very personal choice but one that is best made with all the facts at hand and in consultation with a surgeon whom you trust.
What is fluid on the knee? What is joint effusion?
Everyone has fluid in all mobile joints (hips knees shoulders etc) but usually the amount of fluid is very small (really just enough to coat the surfaces of the joints themselves) and under normal conditions you don't know it's there. The fluid serves two main functions. One function of the fluid is to help lubricate the cartilage surfaces so they move smoothly. In fact normal cartilage that is lubricated by normal joint fluid (called "synovial fluid") is many times more slippery than a hockey puck gliding across a smooth ice rink. The other function of the fluid is to help nourish and protect the cartilage surfaces of the joint.
But when you have enough fluid in a joint to where you notice it (either by being able to see it or by being able to feel it as a tense swelling) that's what people call "water on the joint." The technical term is a "joint effusion." Such a visible or detectable swelling of a joint is never normal and it may be caused by any of a number of conditions including:
- Arthritis: Either osteoarthritis -- called degenerative joint disease -- or inflammatory arthritis such as rheumatoid arthritis
- Trauma: The fluid in certain kinds of trauma may be blood rather than synovial fluid
- Infection: The fluid in this case may be pus rather than synovial fluid
Depending on the cause of the fluid accumulation the treatments may be very different.
It is reasonable to speak to an orthopedic surgeon should you detect water on a joint if that joint is also painful.
Available treatments
Total hip replacement is widely considered one of the most reliable operations devised in the 20th century. The reason for this is that the likelihood of success (and the benefits of a good hip replacement) far outweighs the chance of failure.
However when a hip replacement fails it can be a serious problem. Hip dislocation (when the ball comes out of the socket) is painful and inconvenient. Until the dislocation is reduced (put back in the socket) it is all but impossible to even walk.
The chance that a hip replacement will dislocate varies depending on many circumstances. The likelihood that this complication will occur ranges from less than 1 percent to 10 percent depending on a number of risk factors. But the initial treatment of a first dislocation is typically the same: the patient will be sedated (made sleepy) and by manipulating the joint the ball usually can be put back into the socket. Sometimes this does not succeed and in those cases the hip may need to be surgically opened again and the dislocation treated with an operation to put the ball back in the socket. Sometimes a brace may be worn after a first-time dislocation.
A majority of patients who have one hip dislocation will never have another.
But a significant minority (20-30 percent or more) of patients will re-dislocate either early or later on.
The treatment for someone with multiple (or recurrent) dislocations is nearly always surgery and is geared towards identifying and treating the cause of the dislocation. Common causes include:
- Unsatisfactory position of the component parts of the hip replacement (either the cup or the stem); this is by far the most common problem
- Incorrect soft-tissue tension of or poor functioning of the muscles around the hip
- Impingement (levering) of the thigh bone or the component in it against the pelvis
- Infection
- Severe soft-tissue deficiencies around the hip joint
There are surgical treatments that specifically address each of those causes and sometimes more than one cause is present. There are also specially designed hip implants that by design resist dislocation; however those devices can cause other problems and it is best to avoid using them if possible.
This is a very complex problem and none of the reliable surgical solutions are technically easy to perform. This is reflected in the success rate of surgery which is only about 80 percent in the best of circumstances.
Because of this it is reasonable to seek advice from a surgeon who has particular expertise in the treatment of this difficult problem. Most orthopedic surgeons consider this a challenge best addressed by a joint replacement specialist.
Will a cortisone shot help delay hip or knee replacement?
Cortisone (more properly corticosteroid) injections into joints have been used to relieve arthritis symptoms--including pain swelling and inflammation--for over 50 years. Despite this there have been surprisingly few well-designed scientific studies to determine which patients might benefit from this treatment or how long the relief might last.
Just the same, cortisone shots are commonly used--and often are successful--in helping to relieve arthritis symptoms temporarily. Some patients are able to use them to get enough pain relief to hold off joint replacement surgery for months or even years. Cortisone shots are a treatment for pain; they do not alter the course of arthritis and they do not cure the condition.
Many patients have fears about cortisone shots. Some common ones include:
- Will the cortisone shots cause bone or organ damage? (Answer: no).
- Will cortisone shots cause the arthritis to worsen or otherwise "ruin the joint"? (Answer: in reasonable doses this has not been shown to be a problem, though one study recently suggested that some cartilage thinning was noticeable on MRI tests after joint injections).
- Are they very painful? (Answer: if the person doing the injection is skillful generally not).
Injecting a knee joint with corticosteroids is a relatively straightforward procedure that when done properly takes only a moment and is not too uncomfortable. Relief is nearly immediate because the cortisone usually is mixed with a local anesthetic similar to Novocain used by the dentist; several hours later the corticosteroid preparation will begin to have its anti-inflammatory effects on joint tissues. These effects can last anywhere from several days to 6 months or more. Most commonly the relief lasts several weeks to several months. In view of this many patients opt to try one or more cortisone shots before going ahead with a knee replacement. It is fairly clear that if one or two cortisone shots does not provide a reasonable level and duration of benefit repeated injections are unlikely to be helpful.
In contrast injecting a hip joint is difficult and cannot be done reproducibly in the office setting. In order to make sure the needle will consistently find its way into the joint space of the hip special radiology equipment like an ultrasound or fluoroscopy machine is needed. Having a hip joint injection is much more uncomfortable and inconvenient for the patient than having a knee injection. Also for reasons that are not clear hip joint injections seem not to work as well as knee joint injections. Perhaps for these reasons nearly no research has been done on cortisone shots for hip joint arthritis and most surgeons opt not to do them for the majority of patients with hip arthritis.
In summary the potential advantages of cortisone shots for knee arthritis are:
- They provide rapid onset of pain relief which may last for weeks or months.
- They are not too uncomfortable.
- They are convenient.
The risks of cortisone shots are:
- The risk of infection from putting the needle in the joint (which can be minimized by using careful technique); this risk has been listed as anywhere between 1 in 1000 and 1 in 16000 so the risk is not very great.
- That repeated injections can cause a loss of skin coloration in the area where the shot was placed.
- That occasionally the arthritis can flare up in the hours after a shot; this usually passes over the next day or so. They may result in cartilage thinning, though in the recent study that suggested this the thinning was mild and it was not clear whether this will or will not be a clinical problem.
Like so many things in medicine there are risks and benefits to cortisone shots for knee arthritis. Cortisone shots for hip arthritis are rarely performed.
In any case the best way to find out if this treatment for you would be to discuss it with a hip and knee arthritis specialist.
More information
For more information about hip replacement surgery see this article.
Does hip replacement improve range of motion?
A hip replacement can sometimes improve range of motion.
In general the two main symptoms from hip arthritis are pain and stiffness. Most of the time hip replacement relieves both symptoms although it is much more reliable at relieving pain than it is at restoring range of motion.
Hip motion after total hip replacement though it usually improves rarely returns completely to normal. This is not a terrible problem because one of the feared complications of hip replacement -- where the ball comes out of the socket after surgery called a dislocation -- often happens at the extremes of motion. So failure to regain every bit of normal motion is from that standpoint not so bad.
Even though most patients generally improve their range of motion after hip replacement -- which helps make typical daily activities including intimacy more comfortable -- this is not the case for every patient. Sometimes range of motion will not change after hip replacement or some range will be lost; interestingly this usually is the case in patients with very good range of motion to start with. And rarely a hip can become much stiffer -- or completely immobile -- after a hip replacement. This usually happens because some abnormal bone forms in the soft tissues (called heterotopic ossification) in response to the trauma of surgery itself. Significant activity-limiting stiffness from that condition occurs in perhaps one or two percent of patients after hip surgery and complete loss of motion is extremely rare.
Most of the time motion stays about the same or improves a bit after total hip replacement. And many times a good hip surgeon can predict -- by evaluating a patient for certain risk factors -- whether an individual is likely to form heterotopic ossification around the hip and take measures to prevent post-operative stiffness from this condition.
As always the most important thing to do is to find a surgeon with good experience in hip replacement surgery to help minimize the risks and optimize the benefits from a complex procedure like joint replacement.
The decision to get a hip replacement at any age is a quality of life choice which is made by trying to balance the potential improvement one might get from hip replacement (in terms of decreased pain or restoration of function) against the risks of the procedure. There are certain "generic" risks of hip replacement for patients of any age--infection bleeding nerve injury blood clots hip dislocations leg length inequality persistent pain are a few of these (sounds like lots of risks but usually the actual likelihood of each of those is quite low). But in the case of someone younger than age 50 or so who is otherwise in good health one needs to add at least one additional risk: there is a near-certainty of needing a re-operation (perhaps multiple re-operations) on the hips at some time(s) in one's lifetime. Hip replacements are fairly reliable over the first decade (most research shows that 90% of hip replacements remain in service 10 years after surgery) but there is not expectation for example that they will last the 30-40 years or more that a 40-year-old patient might live. And with each subsequent re-operation the risk of major surgical complications increases.
In general I tell young patients with severe arthritis to try to put up with it as long as they can and when they are no longer able to manage to go ahead with surgery--in full understanding of the risks I mentioned above in particular the very high likelihood of needing more surgery on the affected hip.
This is a very serious and very personal decision. It is a decision best made in concert with a surgeon who specializes in joint replacement who will be able to get to know you well examine you and interpret your X-rays. for more information on hip replacement surgery please visit the article "What is Hip Replacement? A Review of Total Hip Arthroplasty Hip Resurfacing and Minimally-Invasive Hip Surgery"
Surgical options
First of all it is important to recognize how difficult – and how personal – this choice is. The final decision will be made based not only on symptoms physical findings on a surgeon’s exam and the x-ray pattern of arthritis but also on the patient’s goals expectations job demands and level of motivation. For those reasons it is best made in consultation with a subspecialist in adult reconstructive knee surgery and joint replacement.
But by way of summary it is possible to offer the following observations about each of those procedures:
- Unicompartmental Knee Arthroplasty. Although these are now often implanted through a less-invasive surgical approach which can significantly shorten the recovery period unicompartmental knee replacement (“Uni’s”) are a type of joint replacement. As such they really are not meant for people doing impact or twisting sports. Total knee replacements have been studied in patients aged 50 and under and have shown good results in that population with 85-95% of the implants remaining in service 10 years after surgery. By contrast we have fairly limited data on Uni patients of that age group. In most reports of older patients Uni’s have a slightly (but not severely) lower 10-year success rate than total knee replacements. In their favor Uni’s have a much shorter post-op recovery time and most patients find Uni’s perform better and feel more normal than traditional total knee replacements. They also are fairly easily converted to total knee replacements if they should fail. I don't recommend it but I know that some patients have returned to tennis skiing etc after knee replacement surgery (total or uni). That is a personal decision and it needs to be made with the recognition that this likely increases the likelihood of premature failure. There has been a trend towards Uni’s in younger patients in this country because that operation is perceived to be a less-invasive (and more easily revised) approach. But to be honest we don't know if this is going to be a good thing; Unis are now being put into a population of more active patients than they've been really tested in. Only time will tell.
- Total knee arthroplasty (TKA). Long considered the “gold standard” for knee arthritis surgery in older adults (age 60 and over) this operation also is being used more in younger patients in this country. As mentioned there is reasonable clinical follow-up available on TKA’s in patients aged 50 and younger showing that about 9 out of 10 implants remain in service at the end of the first decade; in older patients (age 60 and up) the likelihood is about 95%. TKA’s fail at the rate of about 1 or 1.5% per year on average so it is possible to get at least a ballpark idea of the likelihood of an implant being in service at a particular duration of follow-up. Some patients go back to light doubles tennis and gentle skiing (assuming they were skillful skiers before) but by no means are all patients comfortable doing this and I certainly don’t suggest that my patients do these activities after total knee replacement nor do I promise anyone that they’ll be able to participate in these kinds of sports. The large majority — well over 90% — of patients in this age group are able to return to non-impact exercise (swimming biking or walking) for fitness following this surgery.
- High-Tibial Osteotomy. This operation involves cutting and repositioning one of the bones around the knee joint. This is done to re-orient the loads that occur with normal walking and running so that these loads pass through a non-arthritic portion of the knee. That’s why it doesn’t work well if more than one compartment of the knee is involved--in those patients there is no “good” place through which the load can be redistributed. This may be the operation of choice for people (with the right pattern of arthritis) who want to return to impact sports. However it has some disadvantages. In general pain relief is less dramatic or complete compared to total knee replacement or Uni. Also the likelihood of making 10 years after the surgery without needing another operation (usually a total knee replacement) is much lower than for either of the other operations we’re discussing: only 60-65% of patients who have an osteotomy have gone 10 years without a reoperation. Some surgeons believe that if the arthritis is are already severe (“bone-on-bone”) osteotomy is not likely to be satisfying. Some surgeons say — only half in jest — that the less you need the osteotomy the better you do with it; that is patients with severe arthritis don't do as well as patients with milder disease. Osteotomy also cannot be done in patients whose arthritis has resulted in significant loss of knee joint motion before surgery. In this country there has been a general trend away from osteotomy altogether because of some of the reasons listed aove.
Again this complex and personal choice is best made with some guidance from a subspecialist in adult reconstructive knee surgery and joint replacement. Best of luck!