Edited by Nick Hernandez, M.D., Assistant Professor, UW Orthopaedics & Hip & Knee
Overview
This article covers topics related to unicompartmental knee arthroplasty (sometimes called unicompartmental knee replacement or partial knee replacement) using minimally-invasive surgery (MIS) techniques for the treatment of arthritis.
Knee replacement is a surgical procedure that decreases pain and improves the quality of life in many patients with severe arthritis of the knees. Typically patients undergo this surgery after non-operative treatments (such as activity modification medications knee injections or walking with a cane) have failed to provide relief of arthritic symptoms. Surgeons have performed knee replacements for over three decades generally with excellent results; most reports have ten-year “success rates” in excess of 90 percent.
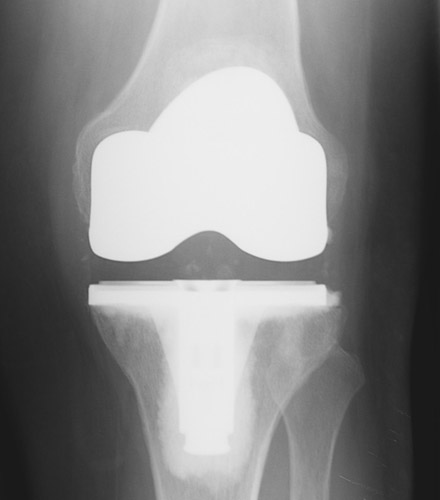
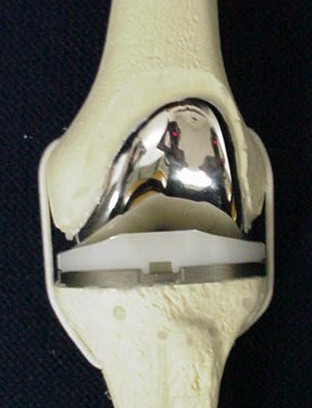
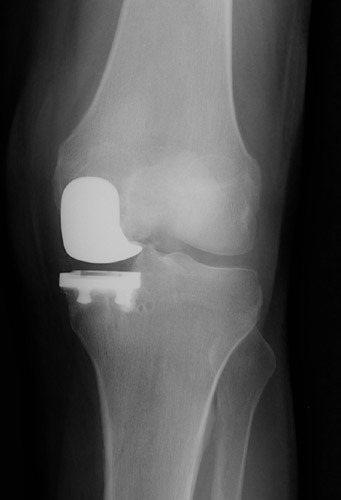
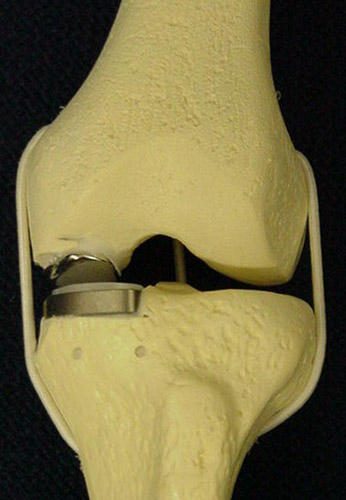
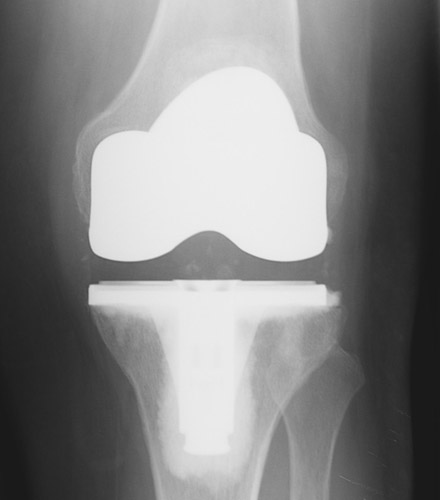
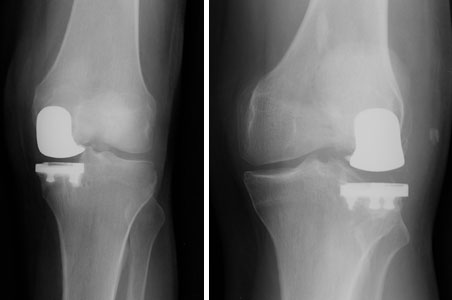
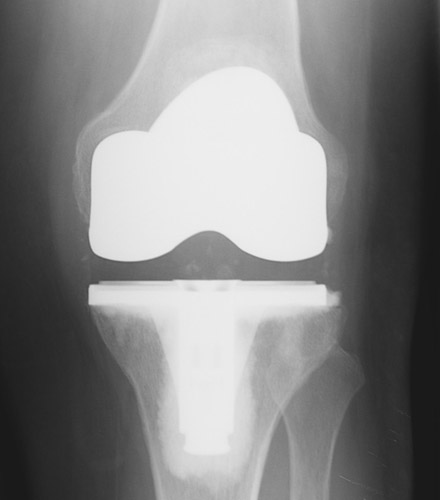
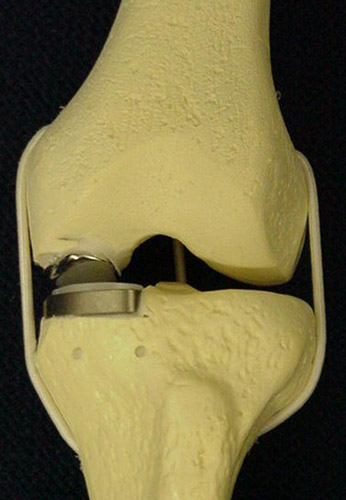
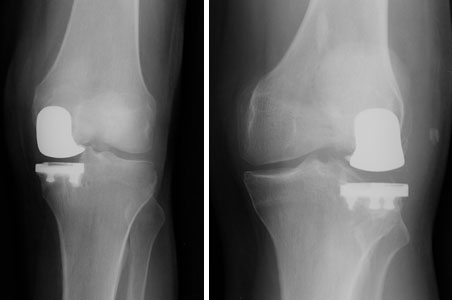
Broadly speaking there are two types of knee replacements: total knee replacements (see figures 1 and 2) and unicompartmental (or partial) knee replacements (see figures 3 and 4). Both have long “track records” and good clinical results in this country and in Europe.
Traditional total knee replacement involves a 7-8” incision over the knee a hospital stay of 3-5 days and a recovery period (during which the patient walks with a walker or cane) lasting from one to three months. The large majority of patients report substantial or total relief of their arthritic symptoms once they have recovered from a total knee replacement.
Partial (unicompartmental) knee replacements have been around for decades and offer excellent clinical results just like total knee replacements.
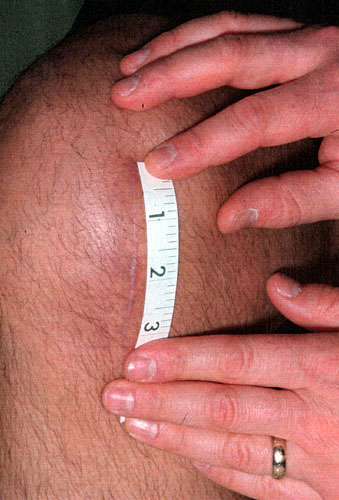
But in the last year or two surgeons and patients have become very enthusiastic about an exciting new approach to this well-established procedure. “Minimally-invasive” partial knee replacement (or "mini knee") is a surgical technique that allows a partial knee replacement to be inserted through a small (3-3.5”) incision (see figure 5) with minimal damage to the muscles and tendons around the knee.
The small size of the incision and the less-invasive nature of the surgical approach allow patients to recover from the “mini knee” operation much more quickly. Hospital stays are shorter--down to 1 or 2 days for most patients--and the recovery period is much faster. Patients lose less blood experience substantially less pain than traditional knee replacement and often walk unassisted (no cane or walker) within a week or two of the operation (see movie 1). Even many patients who have both knees done at once with this newer technique are able to walk without the assistance of a walker or cane fairly quickly.
Patient walking less than 2 weeks after having both knees replaced on the same day
Symptoms & Diagnosis
Characteristics of arthritis of the knee
Pain
Pain is the most noticeable symptom of knee arthritis. In most patients the pain gradually gets worse over time but sometimes has more sudden “flares” where the symptoms get acutely severe. The pain is almost always worsened by weight-bearing and activity. In some patients the pain becomes severe enough to limit even routine daily activities.
Stiffness
Morning stiffness is present in certain types of arthritis; patients with this symptom may notice some improvement in knee flexibility over the course of the day. Rheumatoid arthritis patients may experience more frequent morning stiffness than patients with osteoarthritis.
Swelling and warmth
Patients with arthritis sometimes will notice these symptoms. If the swelling and warmth are excessive and are associated with severe pain inability to bend the knee and difficulty with weight-bearing those signs might represent an infection. Such severe symptoms require immediate medical attention. Joint infection of the knee is discussed below.
Location
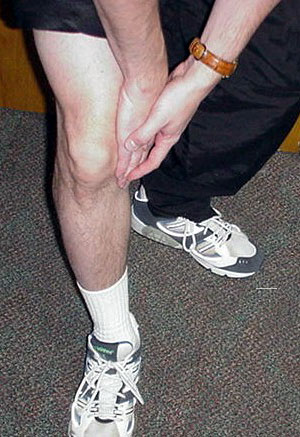
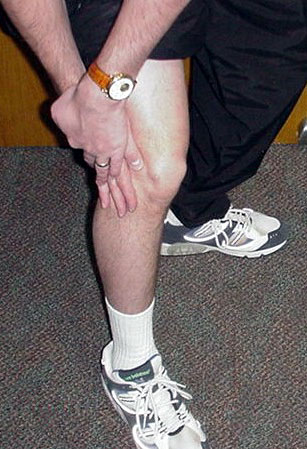
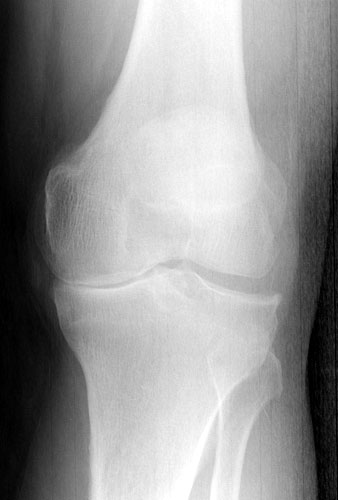
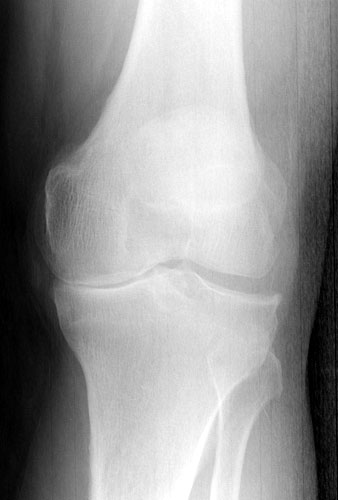
The knee joint has three “compartments” that can be involved with arthritis (see figure 6). Most patients have both symptoms and findings on X-rays that suggest involvement of two or more of these compartments--for example pain on the lateral side (see figure 7) and beneath the kneecap (see figure 8). Patients who have arthritis in two or all three compartments and who decide to get surgery most often will undergo total knee replacement (see figures 9 and 10).
However some patients have arthritis limited to one compartment of the knee--most commonly the medial side (see figure 11). When patients with one-compartment arthritis (also called “unicompartmental” arthritis) decide to get surgery they may be candidates for the mini knee (see figure 12).
Types
Inflammatory arthritis
This broad category includes a wide variety of diagnoses including rheumatoid arthritis, lupus, gout and many others. It is important that patients with these conditions be followed by a qualified rheumatologist as there are a number of exciting new treatments that may decrease the symptoms and perhaps even slow the progression of the joint damage.
Patients with inflammatory arthritis of the knee usually have joint damage in all three compartments and therefore are not good candidates for partial knee replacement. However inflammatory arthritis patients who decide to have total knee replacement have an extremely high likelihood of success; these patients often experience total or near-total pain relief following a well-performed joint replacement.
Osteoarthritis
Osteoarthritis is also called OA or “degenerative joint disease.” OA patients represent the large majority of arthritis sufferers. OA may affect multiple joints or it may be localized to the involved knee. Activity limitations due to pain are the hallmarks of this disease.
OA patients who have symptoms limited to one compartment of the knee are sometimes good candidates for the mini knee.
Similar conditions
Meniscus tear
Sometimes patients with knee pain don't have arthritis at all. Each knee has two rings of cartilage called "menisci" (this is the plural form of "meniscus"). The menisci work similarly to shock absorbers in a car.
Menisci may be torn acutely in a fall or as the result of other trauma or they may develop degenerative tears from wear-and-tear over many years. Patients with meniscus tears experience pain along the inside or outside of the knee; sometimes the pain is worse with deep squatting or twisting. Popping and locking of the knee are also occasional symptoms of meniscus tears.
Since some of these symptoms may be present with arthritis and the treatment of arthritis is different from that of meniscus tears it is important to make the correct diagnosis. A good orthopedic surgeon can distinguish the two conditions by taking a thorough history performing a careful physical examination and by obtaining imaging tests. X-rays and Magnetic Resonance Imaging (MRI) scans may be helpful in distinguishing these two conditions.
Joint infections
Also called infectious arthritis or septic arthritis a joint infection is a severe problem that requires emergent medical (and often surgical) attention. If not treated promptly knee infections can cause rapid destruction of the joint; in the worst cases they can become life-threatening.
Symptoms of a knee joint infection include:
- severe pain
- joint swelling and warmth
- fevers and
- marked inability to walk bend the knee or bear weight.
Patients who suffer from arthritis are not more likely to develop such infections. They may occur in anyone. Arthritis patients who develop such infections would notice a significant worsening in their pain as well as some of the other symptoms listed above.
A physician will make the diagnosis of a joint infection based on history and physical examination blood tests and by sampling joint fluid from the knee.
Again a joint infection is a serious condition that requires immediate medical attention.
Incidence and risk factors
Knee involvement by rheumatoid arthritis (RA) is more common than hip involvement. Approximately 20-30% of patients with RA will have knees affected by this disease.
Diagnosis
History and physical examination
An orthopedic surgeon will begin the evaluation with a thorough history and physical exam. Based on the results of these steps (s)he may order plain X-rays.
X-rays
If you have arthritis of the knee it will be evident on routine X-rays of the joint. X-rays taken with you standing up are more helpful than those taken with you lying down as the way your joint functions under load (i.e. standing) provides important treatment clues to your physician.
Also plain X-rays will allow your orthopedic surgeon to determine whether your arthritis pattern would be suitable for the mini knee should you eventually decide that surgery is for you.
Treatments
Medications
It is important to distinguish broadly between two types of arthritis: inflammatory arthritis (including rheumatoid arthritis lupus and others) and non-inflammatory arthritis (such as osteoarthritis).
Although there is some level of inflammation present in all types of arthritis conditions that fall into the category of true inflammatory arthritis are often very well managed with a variety of medications and more treatments are coming out all the time. Individuals with rheumatoid arthritis and related conditions need to be evaluated and followed by a physician who specializes in those kinds of treatments called a rheumatologist. Excellent non-surgical treatments (including many new and effective drugs) are available for these patients; those treatments can delay (or avoid) the need for surgery and also help prevent the disease from affecting other joints.
So-called non-inflammatory conditions including osteoarthritis (sometimes called degenerative joint disease) also sometimes respond to oral medications (either painkillers like Tylenol or non-steroidal anti-inflammatory drugs like aspirin, ibuprofen, or celebrex) but in many cases symptoms persist despite that type of treatment.
It is important to avoid using narcotics (such as Tylenol #3, vicoden, percocet, or oxycodone) since they are have many side effects are habit-forming and make it harder to achieve pain-control safely and effectively after surgery should that become necessary. Narcotics are designed for people with short-term pain (like after a car accident or surgery) or for people with chronic pain who are not surgical candidates. People who feel they need narcotics to achieve pain control should consider seeing a joint replacement surgeon (an orthopedic surgeon with experience in knee replacements) to see whether surgery is a better option.
Exercises
Once joint destruction of the knee has set in there are no specific exercises that can stop or arrest the development of deformity and joint destruction. Regular range of motion exercises and weight bearing activity are important in maintaining muscle strength and overall aerobic (heart and lung) capacity and help prevent the development of osteoporosis which can complicate later treatment.
Possible benefits of partial knee replacement surgery
This exciting new technique is much less disruptive to the tissues (muscles tendons and ligaments) around the knee than traditional total knee replacement. The small size of the incision and the less-invasive nature of the surgical approach allows patients to recover from this operation much more quickly.
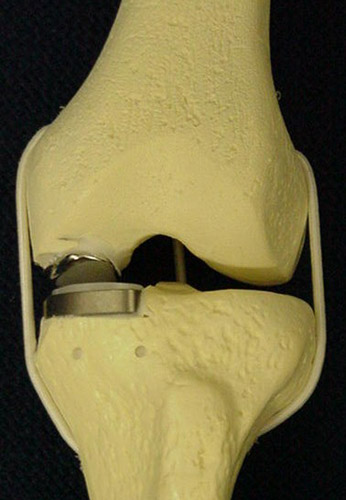
Not all surgical cases are the same, this is only an example to be used for patient education.
Hospital stays are shorter--down to 1 or 2 days for most patients--and the recovery period is much faster. Patients lose less blood experience substantially less pain than traditional knee replacement and often walk unassisted (no cane or walker) within a week or two of the operation. Even many patients who have both knees done at once with this newer technique are able to walk without the assistance of a walker or cane fairly quickly.
A recent study from England (Journal of Arthroplasty Dec 2001; 16(8): 970-6) compared the rehabilitation of minimally-invasive partial knee replacement patients with the rehab of patients who had partial knee replacements done through a longer incision as well as with patients who had conventional total knee replacements. The patients who had the “mini” replacement recovered about twice as quickly as those who had partial replacements done with the older partial-replacement technique and about three times faster than traditional total knee replacements (see video below).
Who should consider partial knee replacement surgery?
It is usually reasonable to try a number of non-operative interventions before considering knee replacement surgery of any type. Prior to surgery your orthopedic surgeon may offer you medications (either non-steroidal anti-inflammatory medications or analgesics like acetaminophen which is sold under the name Tylenol) knee injections or exercises. Your surgeon may talk to you about activity modification weight loss or use of a cane.
The decision to undergo the mini knee is a "quality of life" choice. Patients typically have the procedure when they find themselves avoiding activities that they used to enjoy because of knee pain. When basic activities of daily life--like walking shopping or reasonable recreational pastimes--are inhibited or prevented by the knee pain it may be reasonable to consider the surgery.
What happens without surgery?
Arthritis is often progressive and symptoms typically get worse over time. In some patients the symptoms wax and wane causing “good days and bad days.” Knee arthritis does not usually improve on its own.
Surgical options
If you and your knee surgeon decide that non-operative treatments have failed to provide significant or lasting relief there are sometimes different operations to choose from.
Knee arthroscopy
If your X-rays don’t show very much arthritis and your surgeon suspects (or has identified by MRI) a torn meniscus knee arthroscopy may be for you. This is a relatively minor procedure that is usually done as an outpatient and the recovery is fairly quick in most patients.
However if your X-rays demonstrate a significant amount of arthritis this may not be a good choice. Knee arthroscopy as a treatment for arthritis fails to relieve pain in about half of the patients who try it.
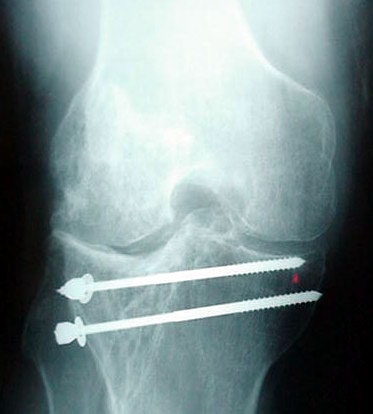
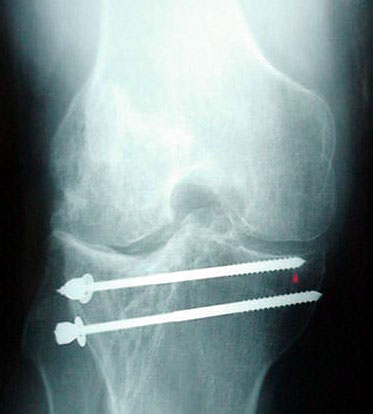
Osteotomy
For younger patients (typically under age 40 but this age cutoff is flexible) who desire to return to a high level of athletic activity or physical work a procedure called osteotomy (which means “cutting the bone”) might be worth considering. This option is suitable only if the arthritis is limited to one compartment of the knee.
Osteotomy involves cutting and repositioning one of the bones around the knee joint. This is done to re-orient the loads that occur with normal walking and running so that these loads pass through a non-arthritic portion of the knee. That’s why it doesn’t work well if more than one compartment of the knee is involved--in those patients there is no “good” place through which the load can be redistributed.
Knee fusion
Knee fusion also called “arthrodesis ” permanently links the femur (thigh bone) with the tibia (shin bone) creating one long bone from the hip to the ankle. It removes all motion from the knee resulting in a stiff-legged gait.
Because there are so many operations that preserve motion this older procedure is seldom performed as a first-line option for patients with knee arthritis. It is sometimes used for severe infections of the knee certain tumors and patients who are too young for joint replacement but are otherwise poor candidates for osteotomy.
Total knee replacement
Long considered the “gold standard” operation for knee arthritis total knee replacement is still by far the most commonly-performed joint replacement procedure (see figures 13). It is most suitable for middle-aged and older people who have arthritis in more than one compartment of the knee (see figures 14 and 15) and who do not intend to return to high-impact athletics or heavy labor. Results of this procedure generally are excellent with 90-95% of total knee replacements continuing to function well more than 10 years after surgery.
Minimally-invasive partial knee replacement ("mini knee")
Patients who are of appropriate age--certainly older than age 40 and older is better--and who have osteoarthritis limited to one compartment of the knee may be candidates for this exciting new surgical technique (see figures 16 17 and 18). Partial knee replacements have been done for over 20 years and the “track record” on the devices used for this operation is excellent. The new surgical approach which uses a much smaller incision than traditional total knee replacement significantly decreases the amount of post-operative pain and shortens the rehabilitation period. The decision of whether this procedure is appropriate for you can only be made in consultation with a skillful orthopedic surgeon who is experienced in all techniques of knee replacement.
Minimally-invasive knee replacement is not for everyone. Only certain patterns of knee arthritis are appropriately treated with this device through the smaller approach.
Generally speaking patients with inflammatory arthritis (like rheumatoid arthritis or lupus) and patients with diffuse arthritis all throughout the knee should not receive partial knee replacements.
Patients who are considering knee replacements should ask their surgeon whether the “mini” partial knee replacement is right for them.
Effectiveness
Current evidence suggests that when partial knee replacements are done well in properly selected patients these procedures have about the same durability as conventional total knee replacements.
Many studies show that more than 90 percent of partial knee replacements are still functioning well 10 years after the surgery. Other research indicates that patients who have a partial knee replacement on one side and a total knee replacement on the other consistently prefer the partial knee replacement. Patients indicate that partial knee replacements feel more “normal” to them when they walk and during typical daily activities.
A recent report demonstrated that the minimally-invasive approach does not interfere with the surgeon’s ability to properly position the joint replacement components within the knee. This is reassuring in terms of the likely long-term performance of partial knee replacements that are inserted using the new technique.
In the event that a partial knee replacement requires re-operation sometime in the future it can be revised to a conventional total knee replacement in a fairly straightforward procedure. Results of that type of revision are usually very satisfactory. In fact revisions of partial knee replacements are typically much easier on both patient and surgeon than revisions of failed total knee replacements.
There is good evidence that the experience of the surgeon correlates with outcome in partial knee replacements. It is important that the surgeon performing the technique be not just an expert knee surgeon but comfortable and experienced with the minimally-invasive technique as well.
Urgency
Minimally-invasive partial knee replacement--much like total knee replacement--is elective surgery. With few exceptions it does not need to be done urgently and can be scheduled around your important life-events.
Risks
Like total knee replacement the mini knee is associated with certain medical and surgical risks. Although major complications are uncommon they may occur; the possibilities include infection blood clots bleeding and anesthesia-related or medical risks. However the overall frequency of major complications following the mini knee is low certainly less than 5 percent (one in 20). Later risks include the possibility that the device may loosen from the bone or that the arthritis may progress and cause pain in other parts of the knee. Studies have shown that when the device is correctly placed in well-selected patients more than 90 percent of these devices remain in service and function well more than 10 years after the surgery--a comparable success rate to total knee arthroplasty. And during that time these devices typically function better than total knee replacements and give patients a more normal “feel” to the knee. Research indicates that patients who have a partial knee replacement on one side and a total knee replacement on the other consistently prefer the partial knee replacement.
Managing risk
Most of the major risks of the mini knee can be treated. The best treatment though is prevention. Your orthopedic surgeon will use antibiotics before during and after surgery to minimize the likelihood of infection. (S)he will take steps to decrease the likelihood of blood clots such as early patient mobilization and use of blood-thinning medications in some patients. Patients are evaluated by a good internist and/or anesthesiologist in advance of the surgery in order to decrease the likelihood of a medical or anesthesia-related complication.
Again the overall likelihood of a severe complication is less than 5 percent when such steps are taken.
Preparation
Patients undergoing mini knee surgery at the University of Washington Medical Center usually will undergo a pre-operative surgical risk assessment. When necessary further evaluation will be performed by an Internal Medicine physician who specializes in pre-operative evaluation and risk-factor modification. Some patients will also be evaluated by an anesthesiologist in advance of the surgery.
Routine blood tests are performed on all pre-operative patients; chest X-rays and electrocardiograms are obtained in patients who meet certain age and health criteria as well.
At the University of Washington surgeons will spend time with the patient in advance of the surgery making certain that all the patient's questions and concerns as well as those of the family are answered.
Costs
The surgeon's office should provide a reasonable estimate of:
- the surgeon's fee
- the hospital fee and
- the degree to which these should be covered by the patient's insurance.
Surgical team
The mini knee requires an experienced orthopedic surgeon and the resources of a large medical center. Patients have complex medical needs and around surgery often require immediate access to a multiple medical and surgical specialties and in-house medical physical therapy and social support services.
Finding an experienced surgeon
There is good evidence that the experience of the surgeon performing partial knee replacement affects the outcome. It is important that your surgeon is not only an experienced knee replacement surgeon; (s)he also should have a high level of skill and experience with the minimally-invasive approach.
Some questions to consider asking your knee surgeon:
- Are you board certified in orthopedic surgery?
- Have you done a fellowship (a year of additional training beyond the five years required to become an orthopedic surgeon) in joint replacement surgery?
- For how long have you been performing the mini knee?
Facilities
A large hospital usually with academic affiliation and equipped with state of the art radiologic imaging equipment and intensive medicine care unit is clearly preferable in the care of patients with knee arthritis.
Technical details
Minimally-invasive partial knee replacement surgery begins by performing a sterile preparation of the skin over the knee to prevent infection followed by inflation of a tourniquet to prevent blood loss during the operation.
Next a well-positioned small incision--approximately 3” in length--is made alongside the kneecap and the knee joint is inspected. It is important at this time to confirm that the arthritis is principally confined to one side of the knee. If there is significant cartilage damage to the undersurface of the kneecap or on the opposite side of the knee a partial knee replacement is unlikely to provide durable pain relief. In those cases a longer incision is then made and a traditional total knee replacement is performed; this change in plans occurs in about 10 percent of patients we consider for partial knee replacement.
This decision to convert from a mini knee to a total knee replacement calls for good judgment and a high level of clinical experience on the part of the surgeon. Proper patient selection is essential for good outcomes in all types of knee surgery but this is especially true for the mini knee.
Next specialized alignment rods and cutting jigs are used to remove enough bone from the end of the femur (thigh bone) and the top of the tibia (shin bone) to allow placement of the joint replacement implants. Proper sizing and alignment of the implants are critical for normal post-operative function and good pain relief. Again these steps are critical and considerable experience in minimally-invasive partial knee replacement is required in order to make sure they are done reliably case after case. Provisional implant components are placed without bone cement to make sure they fit well against the bones and are well aligned; at this time good function--including full flexion (bend) extension (straightening) and ligament balance--is verified.
Finally the bone is cleaned using saline solution and the joint replacement components are cemented into place using polymethylmethacrylate bone cement. The surgical incision is closed using stitches and staples.
Anesthetic
The mini knee may be performed under epidural spinal or general anesthesia. We usually prefer epidural anesthesia since a good epidural can provide up to 48 hours of post-operative pain relief and allow faster more comfortable progress in physical therapy.
Length of partial knee replacement surgery
No two knee replacements are alike and there is some variability in operative times but the average mini knee takes about 75 minutes to perform.
Pain and pain management
One of the principal benefits of the mini knee is that it typically is much less painful than other types of major knee reconstruction.
Whenever possible we use a continuous epidural technique to provide excellent pain relief for the duration of the hospital stay. Patients with a good epidural can expect to walk with crutches or a walker and to take the knee through a near-full range of motion on the day after surgery.
Use of medications
Following discharge from the hospital most patients will take oral pain medications--usually Percocet Vicoden or Tylenol #3--for one to three weeks after the procedure mainly to help with physical therapy and home exercises for the knee.
Quick rehabilitation is the norm following this procedure with most patients being able to walk unassisted between one and two weeks after the surgery.
Effectiveness of medications
Patients who have been through the mini knee on one knee and traditional knee replacement on the other report that the partial knee replacement procedure is much less painful. While any surgical procedure is associated with post-operative discomfort most patients who have had the mini knee say that the pain is not severe and that it is very well controlled with pain medications.
Recovery and rehabilitation in the hospital
Physical therapy starts on the day of surgery in the hospital or the very next day after the operation. Patients are encouraged to walk and to bear as much weight on the leg as they are comfortable doing. Range-of-motion exercises are initiated on the day of surgery or the next morning. The physical therapist should be an integral member of the health care team. In addition the patient’s own high level of motivation and enthusiasm for recovery are very important elements in determining the ultimate outcome.
Hospital discharge
The average hospital stay after the mini knee is two days.
Convalescent assistance
Most patients are able to go home at after two days and do not require any inpatient rehabilitation or other inpatient convalescence following the surgery.
Some patients including the very elderly and those patients who live alone may desire a short stay at an inpatient rehabilitation hospital or extended-care facility; certainly such desires can be accommodated and the necessary arrangements made prior to hospital discharge.
Patients are encouraged to walk and use the knee as normally as possible following the mini knee. Patients are allowed to shower following hospital discharge. We do not recommend that patients drive while taking narcotic-based pain medications; on average patients are able to drive between two and four weeks after the surgery.
Physical therapy
Following hospital discharge patients who undergo the mini knee will participate in either home physical therapy or outpatient physical therapy to a location close to home.
The length of physical therapy varies based upon patient age fitness and level of motivation but usually lasts for 2-4 weeks. Two to three therapy sessions per week are average for this procedure.
At first physical therapy includes range-of-motion exercises and gait training (supervised walking with an assistive device like a cane crutches or walker). As those things become second nature strengthening exercises and transition to normal walking without assistive devices are encouraged.
Can rehabilitation be done at home?
Most patients are discharged from the hospital directly to home and do not require admission to inpatient rehabilitation.
All patients are given a set of home exercises to do between supervised physical therapy sessions and the home exercises make up an important part of the recovery process. However supervised therapy--which is best done in an outpatient physical therapy studio--is extremely helpful and those patients who are able to attend outpatient therapy are encouraged to do so.
For patients who are unable to attend outpatient physical therapy home physical therapy is arranged.
Usual response
Rehabilitation usually proceeds very quickly following the mini knee. Most patients are back to full activities--without the pain they had before surgery--by about a month after the operation.
Risks
This is a safe rehabilitation program with little risk.
Long-term patient limitations
The goal of the mini knee is to return patients to a high level of function without knee pain. The large majority of patients are able to achieve this goal. However since the joint replacement components have no capacity to heal damage from injury sustained after surgery we offer some common-sense guidelines for athletic leisure and workplace activities:
Recommended:
- Swimming
- Water aerobics
- Cross-country skiing or Nordic Track
- Cycling or stationary bike
- Golf
- Dancing
- Sedentary occupations (desk work)
Permitted:
- Hiking
- Gentle doubles tennis
- Gentle downhill skiing
- Light labor (jobs that involve driving walking or standing but not heavy lifting)
Not recommended:
- Jogging or running
- Impact exercises
- Sports that require twisting/pivoting (aggressive tennis basketball racquetball)
- Contact sports
- Heavy labor
Since the joint replacement includes a bearing surface which potentially can wear walking or running for fitness are not recommended. Patients generally feel well enough to do this and so need to exercise judgment in order to prolong the life-span of the implant materials. Swimming water exercises cycling and cross country skiing (and machines simulating it like Nordic Track) can provide a high level of cardiovascular and muscular fitness without excessive wear on the prosthetic joint materials.
Summary of partial knee replacement surgery for arthritis of the knee
Minimally-invasive partial knee replacement (see figure 19) is a surgical technique that allows an artificial knee to be inserted through a small (3 to 3.5 inches) incision (see figure 20) with minimal damage to the muscles and tendons around the knee.
The small size of the incision and the less-invasive nature of the surgical approach allow patients to recover from this operation much more quickly:
- Hospital stays are shorter--down to 1 or 2 days for most patients
- The recovery period is much faster. Most patients can walk unassisted between one and two weeks after the surgery.
- Patients lose less blood than after traditional total knee replacement and rarely require blood transfusions.
- Post-operative pain is experience substantially less pain than traditional knee replacement and the recovery period is much shorter. Even many patients who have both knees done at once with this newer technique are able to walk without the assistance of a walker or cane fairly quickly.