| Last updated: Thursday, February 10, 2005 | ||||||||||||||
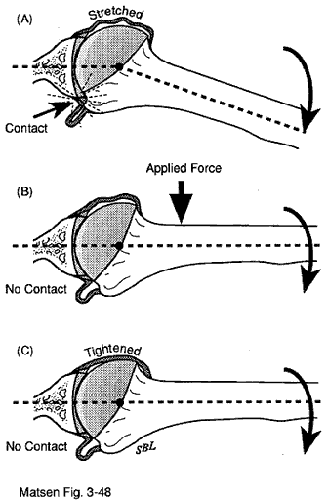
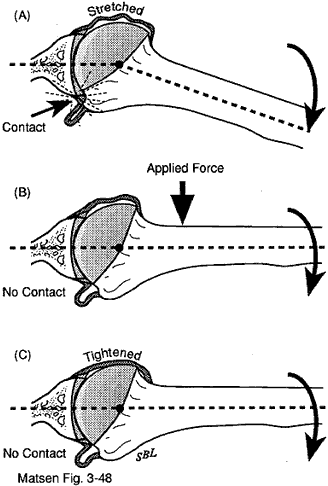
About traumatic instabilitySummary Traumatic instability (TUBS) is instability that arises from an force large enough to injure some of the major supporting structures of the joint, such as the glenohumeral capsule, ligaments, rotator cuff, or the bone of the humerus or glenoid. Usually, traumatic instability arises from a fall on the outstretched hand, for example in skiing, football, or wrestling. In addition to a careful history and clinical examination, X-rays may be helpful in evaluating the patient with traumatic instability. When the instability happens repeatedly or when fear of recurrent dislocation interferes with normal use of the shoulder, surgical repair of the injury can be considered. The postoperative care after this surgery is very important. Movie X-ray of traumatic instability Associated pathologies The most common pathology associated with traumatic instability is the avulsion of the anteroinferior capsule and ligaments from the glenoid rim. Substantial force is required to produce this avulsion in a healthy shoulder. While this load may be applied directly (for example, by having the proximal humerus hit from behind), an indirect loading mechanism is more common. Indirect loading is most easily understood in terms of a simple model of the torques involved. When the upper extremity is abducted and externally rotated by a force applied to the hand, the following equation for torque equilibrium is a useful approximation, if we attribute the major stabilizing role to the ligament: I x R = F x A or equivalently I = F x A/R, where "I" is the tension in the inferior glenohumeral ligament, "R" is the radius of the humeral head, "F" is the abduction external rotation load applied to the hand, and "A" is the distance from the center of the humeral head to the hand. If the radius of the humeral head is 2.5 cm and the distance from the head center to the hand is one meter, this formula suggests that the inferior glenohumeral ligament would experience a load 40 times greater than that applied to the hand. From this example we can see that a much lesser load is required to produce the characteristic lesion of traumatic instability if this load is applied indirectly through the lever arm of the upper extremity. Avulsion of the anterior glenohumeral ligament mechanism deprives the joint of stability in positions where this structure is a major stabilizer of the joint, which is typically approaching maximal external rotation and extension of the arm elevated near the coronal plane. These are positions in which stability is dependent on integrity of the capsuloligamentous mechanism. Thus, it is evident that in recurrent traumatic instability, problems are most likely to occur when the arm is placed in a position approximating that in which the original injury occurred. Midrange instability may also result from a traumatic injury if the glenoid concavity is compromised by avulsion of the labrum or fracture of the bony lip of the glenoid. Lessening of the effective glenoid depth compromises the effectiveness of concavity compression, reduces the angles through which the glenoid can balance the net joint reaction force, reduces the surface available for adhesion-cohesion, and compromises the ability of the glenoid suction cup to conform to the head of the humerus. |
| |||||||||||||
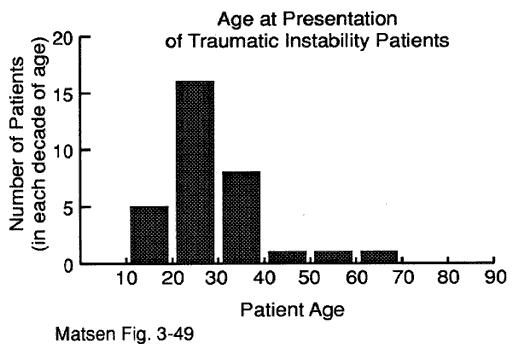
The corner of the glenoid abuts against the insertion of the cuff to the tuberosity when the humerus is extended, abducted, and externally rotated. Thus, the same forces involved in challenging the strength of the inferior glenohumeral ligament are also applied to the greater tuberosity-cuff insertion area. It is not surprising, therefore, that tuberosity fractures and cuff injuries may be a part of the clinical picture of traumatic instability. The exact location and type of traumatic injury depends on the age of the patient and the magnitude, rate, and direction of force applied. Avulsions of the glenoid labrum and glenoid rim fractures are more commonly seen in young individuals after a major injury. In patients over the age of 35, traumatic instability tends to be associated with fractures of the greater tuberosity and rotator cuff tears. This tendency increases with increasing age at the time of the initial traumatic dislocation. Thus, as a rule, younger patients require management of anterior lesions and older patients require management of posterior lesions. The posterior lateral humeral head defect is a common feature of traumatic instability. These lesions are often noted after the first traumatic dislocation and tend to increase in size with recurrent episodes. This impaction injury occurs when the anterior corner of the glenoid is driven into the posterior lateral humeral articular surface. It is evident that this injury is close to the cuff insertion. Large head defects compromise stability by diminishing the articular congruity of the humerus. TUBS syndrome We refer to the usual type of traumatic instability as the TUBS syndrome because it arises from a significant episode of Trauma, characteristically from abduction and extension of the arm elevated in the coronal plane. The resulting instability is usually Unidirectional in the anteroinferior direction. The pathology is usually an avulsion of the capsuloligamentous complex from the anterior inferior lip of the glenoid, commonly referred to as a Bankart lesion. With functionally significant recurrent traumatic instability, a Surgical repair of this ligament avulsion is frequently required to restore function. We have established some diagnostic criteria for making this diagnosis. SLAP lesions SLAP lesions (superior labrum, anterior to posterior) are detachments of labrum (the lining of the glenoid socket of the shoulder). In many cases it is difficult to tell if the labral attachment is normal or not--even with arthroscopy. Thus it is important that the surgeon and the patient be able to relate the symptoms to the finding on arthroscopy. This is a particular challenge because there are no symptoms or presurgical tests that reliably establish the presence of a symptomatic SLAP lesion. Surgery can either trim the labrum or attempt to reattach it. After this surgery, the patient experiences the same type of discomfort as after other arthroscopic surgeries. The details of the recovery and rehabilitation depend on the specifics of the surgery. For example, if there is a trimming, early motion may be carried out, while, after a repair, a period of restricted use may be in order until healing has occurred. | ||||||||||||||
Evaluation and examinationFunctional evaluation Physical examination The goal of the physical examination is largely to confirm the impression obtained from the history: that a certain combination of arm position and force application produces the actual or threatened glenohumeral instability that is of functional concern to the patient. If the diagnosis has been rigorously established from the history, for example by documented recurrent anterior dislocations, it is not necessary to risk redislocation on the physical examination. If such rigorous documentation is not available, however, we must challenge the ligamentous stability of the shoulder in the suspected position of vulnerability. We seek to have the patient identify the positions and events that are of functional significance. The most common direction of recurrent traumatic instability is anteroinferior. Stability in this position is challenged by externally rotating and extending the arm elevated in the coronal plane. This is conveniently done in the supine position with one of the examiner's hands under the back of the shoulder serving as a fulcrum for the external rotation and extension force. We apply extension and external rotation loads in different positions of elevation to challenge the various parts of the anterior capsular mechanism. The patient will very often guard against the position of instability by actively limiting the range of humeroscapular motion. For this reason, we may need to hold the arm in the challenging position for 1 to 2 minutes to fatigue the stabilizing musculature. When the muscle stabilizers tire, the capsuloligamentous mechanism is all that is holding the humeral head in the glenoid. At this moment the patient with traumatic anterior instability becomes apprehensive, recognizing that the shoulder is about to come out of joint. This recognition is strongly supportive of the diagnosis of traumatic anterior instability. Standard tests of glenohumeral laxity are of limited value in the diagnosis of traumatic instability. As has been described earlier the magnitude of translation on the standard test of glenohumeral laxity does not distinguish stable from unstable shoulders. The magnitude of translation on some clinically stable shoulders may be as great or greater than that on shoulders with traumatic instability. However, the experienced examiner may detect certain findings such as increased ease of translation on the anterior drawer test or grinding as the humeral head slides over a bony edge of the glenoid from which the labrum has been avulsed. There may also be a catching or a locking of a torn glenoid labrum, producing findings analogous to those of a torn meniscus in the knee. We do not consider pain on abduction, external rotation and extension to be specific for instability. Such pain may relate to shoulder stiffness or alternatively to abutment of the glenoid against the cuff insertion to the head posteriorly. Furthermore, relief of this pain by anterior pressure on the humeral head may result from diminished stretch on the anterior capsule or from relief of the abutment posteriorly. |
| |||||||||
In all patients with traumatic instability but particularly in those over age 35, the strength of the internal and external rotation must be examined. With increasing age, there is an increasingly common association between traumatic glenohumeral instability and rotator cuff defects. Patients with significant cuff lesions may demonstrate atrophy of the spinatus muscles as well as pain and or weakness on resisted abduction or external rotation. Any rotator cuff pathology must be recognized and incorporated in the treatment plan. Finally, carefully examine the brachial plexus to assure that the episodes of traumatic instability have not compromised its function. Radiographs Radiographs frequently help to provide confirmation of traumatic glenohumeral instability. These findings may include an indentation or impaction in the posterior aspect of the humeral head from contact with the anteroinferior corner of the glenoid when the joint is dislocated. Radiographs may also reveal a periosteal reaction to the ligamentous avulsion at the glenoid lip or occasionally a fracture of the glenoid rim. These lesions are usually revealed by an anteroposterior view in the plane of the scapula, a proper axillary view, and an apical oblique view, as shown in the example movie listed below. We have not found additional radiographic views, CT arthrography, or MRI to be cost effective in the evaluation of shoulders with characteristic traumatic instability. We occasionally use CT to define the magnitude of bone loss when a sizable humeral head or glenoid defects have been identified on a series of plain radiographs. In a patient whose onset of traumatic instability occurred after age 35 there may be evidence on history and physical examination of rotator cuff pathology. In these situations, preoperative imaging of cuff integrity may play an important role in surgical planning: the approach for rotator cuff repair is quite different than the approach for the repair of an anterior inferior capsular lesion. Electromyography may be helpful in the evaluation of the patient with recurrent traumatic instability if the history and physical examination suggest residual brachial plexus lesions. Movie TUBS Radiograph | ||||||||||
TreatmentManagement options A patient with traumatic anterior glenohumeral instability has symptoms of instability (apprehension, subluxation, or dislocation) when the arm is elevated near the coronal plane, extended, and externally rotated. Characteristically the shoulder is relatively asymptomatic in other extreme positions or in midrange positions. Thus, for some patients appropriate management may consist solely of education about the nature of the lesion and identification of the positions and activities that need to be avoided. Strengthening the shoulder musculature may help prevent the shoulder being forced into positions of instability. The exercise program suggested for atraumatic instability may be considered as an option for traumatic instability as well. "Training tape" may be applied to the anterior aspect of the shoulder as a reminder to avoid abduction, external rotation, and extension ofthe shoulder. However, many patients with refractory symptoms will wish to consider surgical repair. |