| Last updated: Wednesday, January 26, 2005 | ||||||
About subacromial smoothingThis is the information which might be shared with patients prior to subacromial smoothing. Before it can be applied to a specific clinical situation, however, it needs to be tailored to the patient, the problem, and the surgeon. Smooth shoulder sliding One of the important aspects of shoulder function is the smooth sliding of the upper arm bone (humerus) and the tendons attached to it (the rotator cuff) beneath an arch made of bone and ligaments. This smooth sliding may be interrupted by changes in the mechanics of the joint, by shoulder tightness, by muscle weakness, or by changes in the bone structure. In most instances much of the function of the shoulder can be regained if you carry out a quality stretching and strengthening exercise program. For shoulders in which a diligent course of quality exercises does not restore a satisfactory level of function, a surgical approach to the area of roughness may be considered. |
| |||||
Who should consider surgery If a persistent and proper rehabilitation effort fails to restore functional humeroscapular smoothness, consideration may be given to a surgical approach to the problem. Surgical smoothing is likely to be of functional benefit only if the patient's functional problem can be clearly localized. This procedure is not appropriate for poorly defined shoulder pain, for cuff strain, for partial thickness cuff tears, or for shoulder stiffness. If stiffness is not resolved preoperatively, subacromial surgery is likely to make the shoulder function worse. We have found that surgical treatment of subacromial roughness is most likely to be successful in a well-motivated patient over the age of 40 whose problem has been refractory to a good home program effort and who has a positive "abrasion" sign: rotation of the arm elevated to the horizontal position reproduces the crepitance that the patient recognizes as the primary problem in his or her shoulder. | ||||||
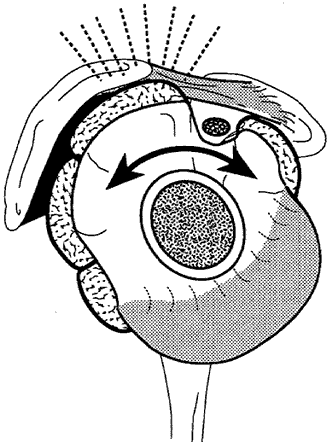
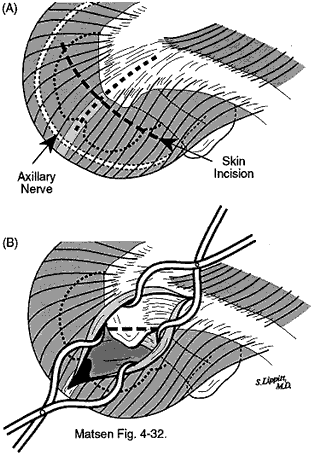
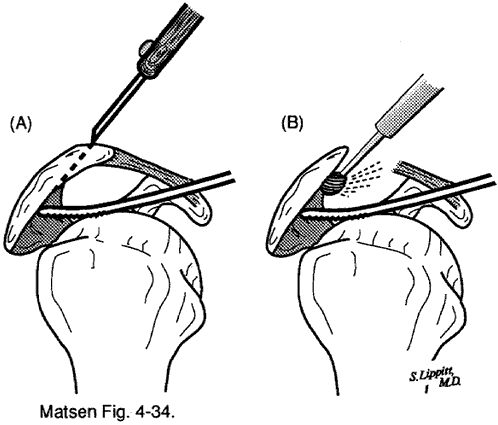
Surgical approachThe surgical approach to roughness in the humeroscapular motion interface must be guided by the location of the problem. Shoulder roughness after previous surgery A shoulder having roughness after previous surgery is generally approached through the previous incision because this provides best access to the postoperative scar. Prior to the incision, the passive motion of the shoulder is verified under anesthesia. If tightness is identified, the approach may need to be modified to allow appropriate surgical releases. Previously unoperated shoulders Previously unoperated shoulders with positive subacromial abrasion signs are approached through an anterior-superior acromioplasty approach. The incision is in the skin lines, crossing the anterior corner of the acromion, and ending just lateral to the coracoid process. The deltoid muscle is split in line with its fibers through the middle of the tendons, separating its anterior and middle thirds, preserving the continuity of the tendinous fibers of origin with the muscle. The subdeltoid bursa on the deep surface of this muscle is entered. Thickened bursa is resected to help smooth the space and to allow inspection of the subjacent rotator cuff. An evaluation of the integrity of the cuff is made at this time. If a cuff defect is present, its reparability is assessed. A traditional acromioplasty with resection of a substantial amount of the anterior inferior acromion and the coracoacromial ligament must be avoided in the presence of a large irreparable rotator cuff defect. This is because the coracoacromial arch provides needed secondary stability when the primary stabilizing function of the cuff is rendered ineffectual. Thus when substantial roughness of the nonarticular humeroscapular motion interface exists in the presence of an irreparable cuff defect, emphasis must be placed on smoothing the contacting surfaces rather than "decompression." Rough edges of the acromion, hypertrophic bursal tissue, prominent tuberosities, previously placed sutures, scar, and irregular edges of cuff tissue are removed to leave the smoothest possible nonarticular humeroscapular motion interface. We perform this smoothing sequentially, putting the arm through a complete range of elevation and rotation, identifying bony contact points and then smoothing them down with a bur or rongeur. This process is continued until smoothness and lack of acromiohumeral contact can be verified in all humeroscapular positions. Smoothness of the motion between the anterior aspect of the subscapularis and the deep surface of the muscles originating from the coracoid process must be verified as well. |
| |||||||||||||
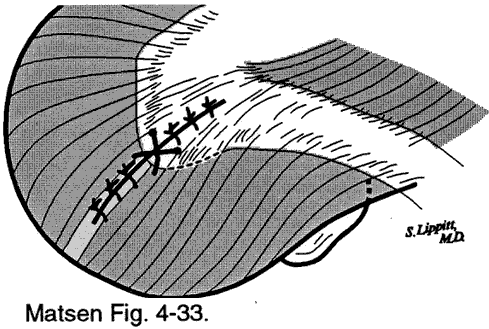
Standard acromioplasty If the rotator cuff is intact or repairable with good quality durable tissue, a standard acromioplasty is performed with resection of the anterior undersurface of the acromion and coracoacromial ligament. Again, the potential areas of contact are examined repeatedly in different positions to assure that adequate smoothness of the undersurface of the coracoacromial arch and the superficial surface of the rotator cuff and humerus has been achieved. Major cuff defects are repaired securely after appropriate releases so that the cuff is under physiologic tension with the arm at the side. Because the primary goal of the procedure is to regain smooth motion, any repair must be sufficiently strong to allow immediate postoperative passive ranging of the shoulder. Again, before closing, the shoulder is put through a complete range of motion to verify smoothness of the nonarticular humeroscapular motion interface, both in the subacromial and coracoid areas. Deltoid repair The deltoid is repaired securely so that immediate postoperative motion can be established. We hypothesize that immediate postoperative passive motion induces the undifferentiated cells in the surgical site to generate a smooth new motion interface, rather than irregular and adherent opposing surfaces. For this reason we use immediate postoperative continuous passive motion in the recovery room and continue it until the patient can carry out his or her mobilization program without assistance. | ||||||||||||||
Failed acromioplastyAt present, "failed acromioplasty" is a very common condition among patients referred to our shoulder service. Complaints Postacromioplasty complaints often include:
Causes of failure These failed open or arthroscopic acromioplasties were usually performed for a preoperative diagnosis listed as "impingement syndrome." However, a careful history often suggests other diagnoses, such as a partially frozen shoulder, cuff strain, partial cuff tears, and nonspecific shoulder pain. Thus these failures seem to be due to:
|