Last Updated: January 25 2005
Diagnosis of shoulder problems
Click to enlarge
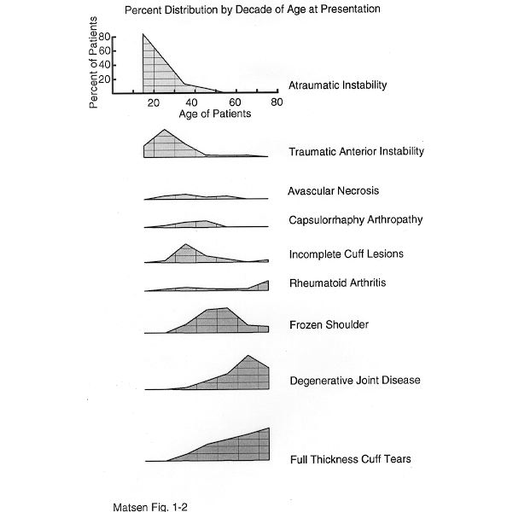
Figure 1 -
Ages different diagnoses
are most prevalent:
the percent distribution
by decade of age
at presentation
of shoulder problems.
Mechanical problems of the shoulder are common. Such problems are often revealed by the answers to some simple questions:
- Is the shoulder stiff: can the arm be put in all normal positions?
- Is the shoulder unstable: does it feel like it is going to pop out or slide out of the socket?
- Is the shoulder weak: does it have the strength to carry out desired activities?
- Is the shoulder rough: does it catch and grind with use?
Non-mechanical problems
There is another group of shoulder problems which is not related to shoulder mechanics. These include conditions such as arthritis of the neck nerve irritation bone infection bone tumors and various pain syndromes. These conditions typically produce pain whether or not the shoulder is being used. Persistent non-mechanical problems of the shoulder require a thorough evaluation which is not covered here.
Shoulder problems and age
Certain conditions are most common during certain times in our lives. Based on the ages at which patients present to the University of Washington Shoulder and Elbow Service we can show graphically at which ages the different diagnoses are most prevalent. The youngest ages are dominated by problems of traumatic anterior instability and atraumatic instability. The middle ages includes all the major diagnoses. The older ages are dominated by degenerative joint disease cuff tears and frozen shoulders. Diagnoses other than instability are uncommon under the age of 30. Complete cuff tear are rare under the age of 30.
Conditions without definitive treatments
While we are used to thinking that every clinical problem has a diagnosis and every diagnosis has a treatment this is not the case for the shoulder. Although many shoulder conditions can be managed well a group of shoulder problems exists that are diagnoseable but are not amenable to definitive treatment. Examples include such diagnoses as brachial neuritis habitual dislocations mid-substance muscle tears anterior sternoclavicular subluxation generalized ligamentous laxity instability from movement disorders and massive rotator cuff tears in individuals with paraplegia. In these situations the effectiveness of existing treatment methods is limited. The available resources can be directed to patient education exercises and vocational rehabilitation.
Conditions that are difficult to diagnose
Some shoulder complaints are not even diagnoseable no matter how many tests are ordered. An unlimited amount of resources can be spent in vain pursuit of a treatable cause for vague shoulder problems. A risk in ordering diagnostic tests when the basic evaluation suggests no shoulder pathology is that these tests may yield "findings" which do not relate to the individual's complaint. Findings of "labral fraying" on arthroscopy "abnormal signals in the cuff tendons" on MRI or "laxity" on examination under anesthesia do not help in the evaluation or management of nonspecific shoulder complaints.
From the standpoint of resource allocation it is important to define which shoulder problems do not need expensive diagnostic evaluations. A good guideline is that when the basic evaluation (a careful history and physical examination along with appropriate plain radiographs) does not suggest the existence of a definable problem one need not proceed to advanced imaging electrodiagnostics arthroscopy or examination under anesthesia because the yield is so low under these circumstances. A repeat clinical examination after several months often provides additional insight into the nature of the problem. The diagnosis for "shoulder pain without identified pathology" should be just that. Assigning a label with minimal therapeutic significance such as fibromyalgia myofasciitis or trigger points does not help determine a curative treatment. Usually these situations can best be managed by shifting the expenditure of resources from evaluation to a program of physical vocational and social support.