Last Updated: December 13, 2013
Follow Dr. Matsen's Shoulder Arthritis blog
On which we try to provide the best and most current information on shoulder arthritis.
The patient with significant glenohumeral arthritis usually presents with pain and loss of function which are refractory to rest antiinflammatory medications and exercises. The history should include a description of the onset of the problem the mechanism of any injuries and the nature and progression of functional difficulties. Systemic or polyarticular manifestations of sepsis degenerative joint disease or rheumatoid arthritis may provide helpful clues. A past history of steroid medication fracture or working at depths may suggest the diagnosis of avascular necrosis. Past injury or surgery suggest the possibility of secondary arthritis or capsulorrhaphy arthropathy.
Standardized assessment methods
Recently standardized methods have been developed by which patients can assess their health status and shoulder function. Bostrom et al (Bostrom Harms-Ringdahl Nordemar 1991) found that standardized assessments of shoulder function more reliable and reproducible than conventional range of motion measurements. Matsen et al reported the self assessment of 103 patients with primary glenohumeral degenerative joint disease. (Matsen Lippitt Sidles et al. 1994; Matsen Ziegler and DeBartolo 1995) Over half reported that their SF 36 pain and physical role function scores were more than one standard deviation below those of age and sex-matched controls. These patients consistently reported the inability to perform standard shoulder functions such as sleeping comfortably lifting 8 pounds to shoulder height washing the back of the opposite shoulder throwing overhand and tucking in a shirt behind. Smith et al used self assessment of shoulder function and health status to compare patients with rheumatoid arthritis and degenerative joint disease of the shoulder. (Matsen Smith DeBartolo et al. 1996)
Physical examination often reveals mild or moderate muscle wasting about the shoulder crepitus on joint motion and limited range of motion. The limitation of glenohumeral motion is most easily identified if one of the examiner's hands is used to stabilize the scapula while the flexion/extension and internal/external rotation of the humerus relative to the scapula are documented with the other.
Thorough evaluation is essential
It is important to emphasize that shoulder arthritis may co-exist with other medical conditions many of which will substantially alter the patient's disability and their potential to respond positively to treatment. Thus a thorough evaluation of each individual is essential.
The SF 36 provides a standardized documentation of the patient's self-assessed health status. The importance of factors such as the SF 36 scales of emotional role function mental health and social function is well demonstrated in the work of Summers et al (Summers Haley Reveille et al. 1988) who found that the objective severity of the disease showed little relationship to patients' reports of pain whereas psychological variables were much more closely correlated with measures of pain and functional impairment.
In the evaluation of glenohumeral arthritis standardized radiographic views are necessary to understand the disease process and its severity.
Standard views
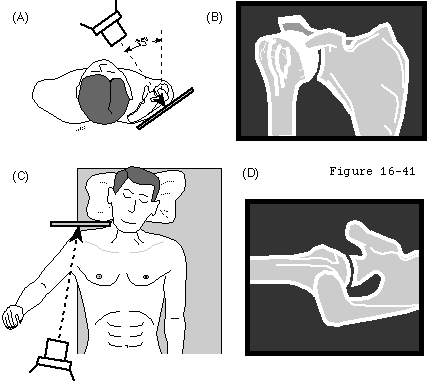
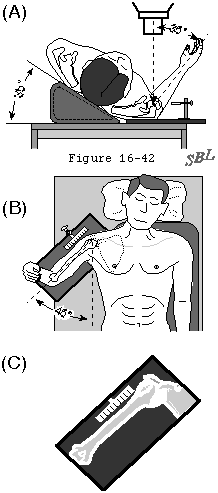
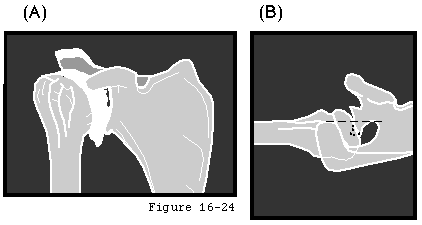
Standard views include an anteroposterior view in the plane of the scapula and a true axillary view (see figure 1). These views indicate the thickness of the cartilage space between the humerus and glenoid the relative positions of the humeral head and glenoid the presence of osteophytes the degree of osteopenia and the extent of bony deformity and erosion. Superior displacement of the humeral head relative to the scapula suggests major cuff deficiency and argues against the use of a glenoid prosthesis (see figure 2). If a humeral arthroplasty is being considered a templating AP view of the humerus in 35 degrees of external rotation relative to the x-ray beam with a magnification marker is obtained (see figure 3). This view places the humeral neck in maximal profile allowing comparison of the proximal humeral anatomy to that of various humeral prostheses. If this view is taken with the arm in 45 degrees of abduction placing the middle of the humeral articular surface in the middle of the glenoid fossa it can reveal thinning of the central aspect of the humeral articular cartilage typical of degenerative joint disease (the "Friar Tuck" pattern) whereas radiographs with the arm in other positions may suggest the presence of a thicker layer of cartilage at the periphery of the head.
CT scans are obtained if there is question about the amount or quality of bone available for reconstruction. Most often these questions can be answered from plain radiographs alone. Friedman et al (Friedman Hawthorne and Genez 1992) and Mullaji et al (Mullaji Beddow and Lamb 1994) have used CT to characterize the changes in version in a group of patients with degenerative and inflammatory arthritis. The most important conclusion from these two studies is that glenoid version varies through a range of 30 degrees in these populations! Mallon et al (Mallon Brown Vogler et al. 1992) have also conducted detailed studies of the articular surface of the glenoid and related this shape to the anatomy of the scapula.
Imaging of the rotator cuff by arthrography MRI or ultrasound is carried out if it will affect management of the patient. Usually the status of the rotator cuff can be understood from evaluation of the history the physical examination and the plain radiographs.
Green and Norris (Green and Norris 1994a) and Slawson et al (Slawson Everson and Craig 1995) have recently provided a review of imaging techniques for glenohumeral arthritis and for glenohumeral arthroplasty.
A number of different processes can destroy the glenohumeral joint surface.
Establishing criteria
Clinical evaluation management and effectiveness measurement is facilitated by establishing necessary and sufficient criteria which enable us to standardize the assignment of each diagnosis. Six of the more common types of glenohumeral joint destruction include: primary degenerative joint disease secondary degenerative joint disease rheumatoid arthritis cuff tear arthropathy capsulorrhaphy arthropathy and avascular necrosis.
In an extension of a recent study on self-assessment of patients with glenohumeral osteoarthritis (Matsen Ziegler and DeBartolo 1995) patients presenting with these conditions assessed their shoulder function using the 12 questions of the Simple Shoulder Test. (Matsen Lippitt Sidles et al. 1994) These individuals with glenohumeral arthritis had greatest difficulty with overhand throwing sleeping comfortably on the affected side washing the back of the opposite shoulder and placing eight pounds on a shelf. Interestingly the degree of functional compromise at the time of presentation for evaluation was comparable for the different diagnoses. Apparently it is this level of functional impairment irrespective of the diagnosis that brings the patient in for evaluation.
These individuals also assessed their health status using the SF 36 (see footnote 1). The self-assessed overall health status of individuals with glenohumeral arthritis is most compromised in the domains of physical role function and overall comfort. For patients with primary and secondary degenerative joint disease and cuff tear arthropathy the other SF 36 parameters such as vitality and overall health were relatively close to population-based age and sex matched controls. The health status of patients with rheumatoid arthritis capsulorrhaphy arthropathy and avascular necrosis was poorer than controls of the same age and sex.
Footnotes
Footnote 1: The SF 36 is a general health status self-assessment used in many fields of medicine.(Radosevich Wetzler and Wilson 1994; Ware Snow Kosinski et al. 1993) It is very useful in orthopedics for documenting the general health deficits of patients before and after reconstructive surgery. The overall comfort and physical role function scales are most commonly affected by arthritic conditions of the shoulder. Other SF 36 scores are useful in documenting the patients' vitality mental health general health and social emotional and physical function.
Primary DJD
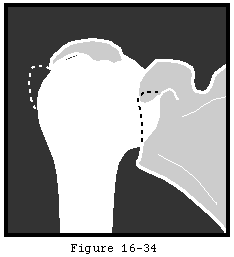
In degenerative joint disease (DJD) the glenoid cartilage and subchondral bone are typically worn posteriorly often leaving intact articular cartilage anteriorly (see figure 4). The cartilage of the humeral head is eroded in a "Friar Tuck" pattern of central baldness often surrounded by a rim of remaining cartilage and osteophytes. Degenerative cysts may occur in the humeral head or glenoid. Osteophytes typically surround the anterior inferior and posterior aspects of the humeral head and the inferior and posterior glenoid. As a result the humeral and glenoid articular surfaces have a flattened configuration which blocks rotation. Loose bodies are often found in the axillary or subscapularis recesses. The triad of anterior capsular contracture posterior glenoid wear and posterior humeral subluxation is common in primary degenerative joint disease. Rotator cuff defects are uncommon in primary degenerative joint disease.
Secondary DJD
In contrast to primary degenerative joint disease secondary degenerative joint disease arises when previous injury surgery or other condition affects the joint surface precipitating its degeneration. In chronic unreduced dislocations (Hawkins Neer Pianta et al. 1987; Pritchett and Clark 1987; Rowe and Zarins 1982) the humeral head may be indented and worn. The cartilage of the joint surfaces may be replaced with scar or the subchondral bone may be so weakened by bone atrophy that it will collapse after reduction leading to an incongruous joint surface. Samilson (Samilson and Prieto 1983) identified seventy-four shoulders with a history of single or multiple dislocations that exhibited radiographic evidence of glenohumeral arthritis. The dislocations had been anterior in sixty-two shoulders posterior in eleven and one had multidirectional instability. The number of dislocations was not related to the severity of the arthrosis. Shoulders with posterior instability had a higher incidence of moderate or severe arthritis as did shoulders with previous surgery in which internal fixation devices intruded on the joint surface. Hawkins and his co-workers (Hawkins Neer Pianta et al. 1987) have suggested hemiarthroplasty if the dislocation is greater than six months old or if the humeral head defect involves more than 45% of the articular surface. If the glenoid is destroyed a total shoulder arthroplasty may be indicated.
Tanner and Cofield reviewed twenty-eight shoulders with chronic fracture problems requiring prosthetic arthroplasty. (Tanner and Cofield 1983) Sixteen had malunions with a joint incongruity eight had post-traumatic osteonecrosis and four had nonunion of a surgical neck fracture with a small osteopenic head fragment.
Shoulders with secondary degenerative joint disease often present complex pathology and difficult surgical management. (Huten and Duparc 1986; Neer and Kirby 1982) Difficulties may be related to a number of factors: muscle contracture scarring malunion requiring osteotomy nonunion or bone loss especially humeral shortening. Dines et al (Dines Warren Altchek et al. 1993) recently reported their results with shoulder arthroplasty in twenty patients with posttraumatic changes. They emphasize the difficulty of these cases and the advisability of avoiding tuberosity osteotomy. Other series of arthroplasty for late sequelae of trauma include that of Norris et al (Norris Green McGuigan 1995) Habermeyer and Schweiberer (Habermeyer and Schweiberer 1992) and Frich et al (Frich Sojbjerg and Sneppen 1991).
Rheumatoid arthritis is a systemic disease with highly variable clinical manifestations. It may be isolated to the glenohumeral joint or may affect most of the tissues in the body.
Effects of arthritis
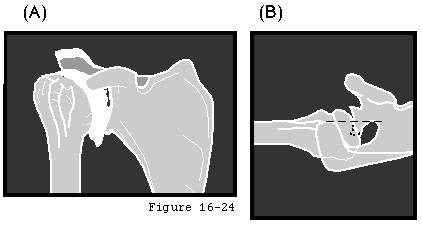
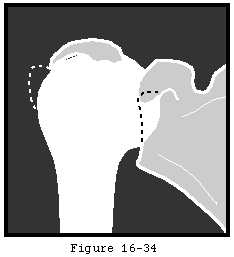
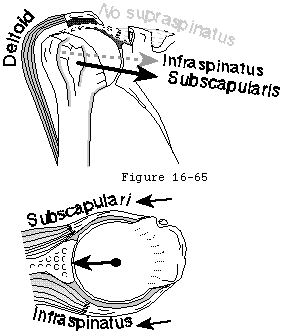
In rheumatoid and many other types of inflammatory arthritis the cartilage is characteristically destroyed evenly across all joint surfaces. The glenoid is eroded medially (see figure 5) rather than posteriorly as in degenerative joint disease (see figure 6). The condition is often bilaterally symmetrical. The arthritic process erodes not only the cartilage but also the subchondral bone and renders it osteopenic. The glenohumeral acromioclavicular sternoclavicular elbow wrist and hand articulations may all be affected greatly amplifying the resulting functional losses. Soft tissues including the rotator cuff may likewise be swollen contracted weakened or torn.
In a clinical and arthrographic study of 200 painful shoulders in patients with rheumatoid arthritis Ennevarra found only 26 per cent of patients had full-thickness rotator cuff defects. (Ennevaara 1967) In two series of patients with rheumatoid arthritis that required total shoulder arthroplasty the rotator cuff had full-thickness tearing in 29 of 69 shoulders (42%) and in 18 of 66 shoulders (27%). (Cofield 1983b; Neer and Kirby 1982)
Even the skin may be fragile and subject to compromise in wound healing. The fragility of the patient with rheumatoid arthritis is frequently compounded by long term use of steroids and other antimetabolic medication. Because the condition itself involves the immune system because the patient is often on immunosuppressive medication and because the clinical manifestations of rheumatoid arthritis are similar to those of infectious arthritis the physician must be aware of the possible coexistence of joint infection.
Petersson (Petersson 1986a) pointed to the prevalence and progression of rheumatoid involvement of the shoulder. Winalski and Shapiro(Winalski and Shapiro 1991) and Mulliaji et al (Mullaji Beddow and Lamb 1994) used computerized tomography to characterize the rheumatoid involvement of the sternoclavicular and glenohumeral joints. Alasaarela and Alasaarela (Alasaarela and Alasaarela 1994) have used ultrasonography to define the soft tissue changes associated with rheumatoid arthritis of the shoulder.
Other conditions
Other conditions may produce shoulder findings quite similar to those of rheumatoid arthritis. Included in the list are localized processes such as pigmented villonodular synovitis (Dorwart Genant Johnston et al. 1984a; Dorwart Genant Johnston et al. 1984b) synovial chondrometaplasia (Hjelkrem and Stanish 1988) and pseudogout. (Hughes Biundo Scheib et al. 1990) The shoulder may be a site of manifestation of systemic disorders such hemophilia and hemachromatosis (Epps 1983; Rand and Sim 1981) primary hyperparathyroidism (Nussbaum and Doppman 1982) acromegaly (Podgorski Robinson Weissberger et al. 1988) amyloid arthropathy (Curran Ellman and Brown 1983) gout (Ellman and Curran 1988) chondrocalcinosis (Cosendai Gerster Vischer et al. 1976) ankylosing spondylitis (Fournie Railhac Monod 1987; Marks Barnett and Calin 1983) psoriasis (Fournie Railhac and Monod 1987) and Lyme arthritis. (Curran Ellman and Brown 1983) Recently Sethi et al (Sethi Naunton-Morgan Brown et al. 1990) have reported a "dialysis arthropathy" which affects multiple joints including the shoulder in individuals on long term dialysis.
Because of the fragility of the skin and other soft tissues the osteopenia and the severe bony erosion common with this condition the patient with substantial involvement from rheumatoid or similar types of arthritis needs to be treated with extreme gentleness thoroughness and care. These admonitions are referred to as "rheumatoid rules."
In a recent review Sneppen et al (Sneppen Fruensgaard Johannsen et al. 1996) pointed to the challenges of arthroplasty in rheumatoid disease. In their series of Neer arthroplasties at 92 month followup 55% showed proximal migration of the humerus relative to the glenoid 40% showed progressive loosening of the glenoid component 5 of 12 press fit humeral components showed progressively loosening (but none in 50 cemented humeral components). In spite of these problems 89% of the patients demonstrated good pain relief. Boyd et al (Boyd Aliabadi Thornhill 1991) found that of 111 Neer total shoulders with an average followup of 55 months progressive proximal migration occurred in 22% of patients (29 shoulders).
Individuals with rheumatoid arthritis characteristically have substantially lower self-assessed vitality and overall physical function than the other causes of glenohumeral arthritis. The compromised general health and strength of individuals with rheumatoid arthritis must be considered in their management as has been emphasized by a recent comparison study of RA and DJD conducted by Smith et al. (Matsen Smith DeBartolo et al. 1996)
About cuff tear arthropathy
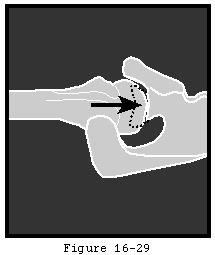
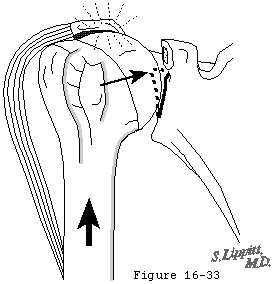
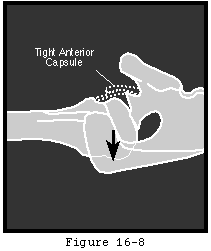
Cuff tear arthropathy occurs when a chronic massive rotator cuff defect subjects the uncovered humeral articular cartilage to abrasion by the undersurface of the coracoacromial arch (see figure 7). The humeral head becomes femoralized and the coracoacromial arch acetabularized (see figure 8). The erosion of the humeral articular cartilage begins superiorly rather than centrally as is the case in degenerative joint disease and capsulorrhaphy arthropathy.
In 1981 McCarty and co-workers described a shoulder condition: the "Milwaukee shoulder." This included significant rotator cuff disease and shoulder arthritis in older patients often women. (Garancis Cheung Halverson et al. 1981; Halverson Cheung McCarty et al. 1981; McCarty Halverson Carrera et al. 1981) The synovial fluid contained aggregates of hydroxyapatite crystals active collagenase and neutral protease. At that time these authors hypothesized that the crystals within the synovial fluid were phagocytized by the macrophage-like synovial cells and the cells in turn released enzymes resulting in damage of the joint and joint-related structures. The inciting process could not be identified.
In 1983 the hypothesis was further refined. The crystals were identified as basic calcium phosphate (BCP). (McCarty 1983) It was thought these crystals would form in the synovial fluid by unknown mechanisms. They would then be phagocytosed by the synovial lining cells. These cells would then secrete the collagenase and neutral protease. This would damage the tissues and in addition cause the release of additional crystals. The importance of this concept may be a more universal understanding of crystal-related arthropathies and a better understanding of how multiple joint structures can be affected by an underlying problem. (Halverson Cheung McCarty 1982; Halverson Garancis McCarty 1984; Halverson McCarty Cheung et al. 1984; Klimaitis Carroll and Owen 1988)
Nguyen and Nguyen (Nguyen and Nguyen 1990) and Campion (Campion McCrae Alwan et al. 1988) have described an "idiopathic destructive arthritis" of the shoulder which may be another form of the same condition.
In 1983 Neer and co-workers published an article on cuff tear arthropathy describing pathological changes in 26 patients. (Neer Craig and Fukuda 1983) These changes included massive rotator cuff tearing glenohumeral instability loss of articular cartilage of the glenohumeral joint humeral head collapse and related bone loss. This entity was distinctly different from osteoarthritis which he had defined earlier. Neer felt that mechanical factors associated with extensive rotator cuff tearing played a prominent role in the creation of this problem and that secondary nutritional changes may augment the pathological changes that occur.
The relationship between &"Milwaukee shoulder" syndrome crystal deposition arthritis and cuff tear arthropathy is unclear. They may be the same process or different process with similar end stages. For the surgeon however the challenge is an eroded joint lacking normal bone stock and lacking reconstructable rotator cuff tissue. In this condition the glenohumeral joint is deprived of several of its major stabilizing factors:
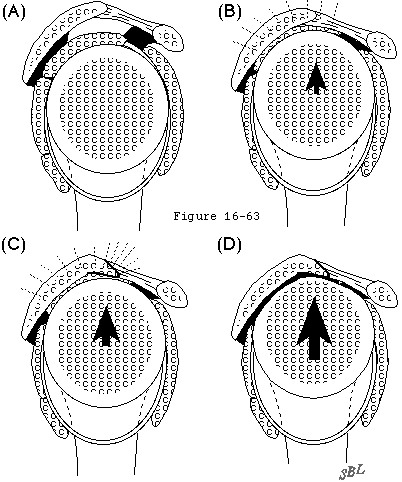
- The normal cuff muscle force vector compressing the humeral head into the glenoid (see figure 9).
- The superior lip of the glenoid concavity which is typically worn away by chronic superior subluxation (see figure 10).
- The cuff tendon interposed between the humeral head and the coracoacromial arch (see figure 11).
As a result of these deficits the superior instability is of sufficient severity that it cannot be reversed in a dependable way at the time of reconstructive surgery.
Arntz et al (Arntz Jackins and Matsen 1993) reported their results from 21 shoulders with cuff tear arthropathy. These shoulders were not candidates for glenoid replacement because of the massive deficiency in the cuff and the fixed upward displacement of the humeral head. Thus they were treated with a special hemiarthroplasty allowing the prosthesis to articulate with the coracoacromial arch. The prerequisites for successful hemiarthroplasty were an intact deltoid and a functionally intact coracoacromial arch to provide superior secondary stability for the prosthesis. One important aspect of the operative technique was the selection of a sufficiently small prosthesis so that excessive tightness of the posterior aspect of the capsule could be avoided. Eighteen shoulders in sixteen patients were available for follow-up which ranged from twenty-five to 122 months. Pain decreased from marked or disabling in fourteen shoulders preoperatively to none or slight in ten and to pain only after unusual activity in four. Active forward elevation improved from an average of 66 degrees preoperatively to an average of 109 degrees postoperatively. One patient who had an excellent result fell and sustained an acromial fracture so the functional result changed to poor. Three patients had persistent substantial pain in the shoulder that led to a revision. Neither infection nor prosthetic loosening developed in any shoulder. Capsulorrhaphy arthropathy is recognized as a special subset of secondary degenerative joint disease in which deterioration of the joint surface related to a previous repair for recurrent dislocations.
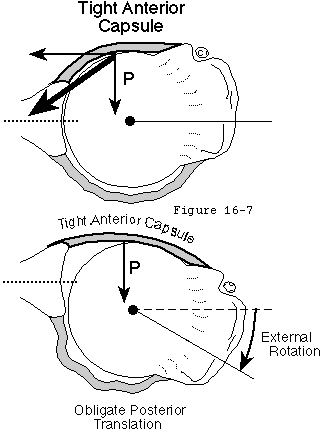
Common cause of arthritis
This is one of the commonest causes of severe arthritis in the individual under fifty-five years of age. Capsulorrhaphy arthropathy may be caused by overtightening the anterior capsule for example in a Putti Platt repair limiting external rotation and causing obligate posterior translation forcing the humeral head out of its normal concentric relationship with the glenoid fossa (see figures 12 and 13). The posterior glenoid is typically eroded from this chronic posterior humeral subluxation; occasionally major posterior bone deficiencies result (see figure 13). The converse situation may arise when obligate anterior translation results from excessive posterior capsular tightening. Lusardi et al (Lusardi Wirth Wrutz et al. 1993) reported a retrospective study of 20 shoulders in 19 patients who had been managed for severe loss of external rotation of the glenohumeral joint after a previous anterior capsulorrhaphy for recurrent instability. All patients had noted a restricted range of motion and 17 shoulders had been painful. In 7 shoulders the humeral head had been subluxated or dislocated posteriorly and 16 shoulders had been affected by mild to severe glenohumeral osteoarthrosis. All 20 shoulders were treated with a reoperation which consisted of a release of the anterior soft tissue. In addition eight shoulders had a total arthroplasty and one had a hemiarthroplasty. At an average duration of follow up of 48 months all shoulders had an improvement in the ratings for pain and range of motion. The average increase in external rotation was 45 degrees.
Capsulorrhaphy arthropathy may also be related to intraarticular positioning of metallic internal fixation devices (screws or staples) or bone graft used in repairs of recurrent instability. (Zuckerman and Matsen 1984)
Bigliani et al (Bigliani Weinstein Glasgow et al. 1995) and Hawkins (Hawkins and Angelo 1990) reported their results from reconstruction of shoulders damaged by capsulorrhaphy arthropathy.
Nontraumatic avascular necrosis of the humeral head may be idiopathic or associated with the systemic use of steroids dysbaric conditions transplantation or systemic illnesses with vasculitis.
Other implicated conditions
Other implicated conditions include alcoholism sickle cell disease hyperuricemia Gaucher's disease pancreatitis familial hyperlipidemia renal or other organ transplantation and lymphoma. (Bradford Szalapski Sutherland et al. 1984; Cruess 1976; Cruess 1985; Rossleigh Smith Straus et al. 1986)
The pathology may first be detected by magnetic resonance imaging before collapse is seen radiographically. Later osteoporosis and/or osteosclerosis may be seen on plain radiographs. Next there is evidence of a fracture through the abnormal subchondral bone superior-centrally. Later collapse of the subchondral bone occurs often with a separated osteocartilaginous flap. In end-stage avascular necrosis the irregular humeral head destroys glenoid articular cartilage resulting in secondary degenerative joint disease. (Cruess 1976; Rutherford and Cofield 1987)
Types
Neurotrophic arthropathy arises in association with syringomyelia diabetes or other causes of joint denervation. The joint and subchondral bone are destroyed because of the loss of the trophic and protective effects of its nerve supply. It has been suggested that the injection of corticosteroids may contribute to the development of this condition. (Parikh Houpt Jacobs et al. 1993) The Charcot joint presents with functional limitation and pain (in spite of the denervation). Cervical spine trauma may have occurred in the past (Rhoades Neff Rengachary et al. 1983) or unrecognized syringomyelia may exist.(Mau and Nebinger 1986; Tully and Latteri 1978) There is usually significant bone destruction and with osseous debris about the joint area. This condition may resemble infectious arthritis. (Louthrenoo Ostrov Park et al. 1990)
Radiation therapy especially for the treatment of breast cancer may cause a number of shoulder problems: brachial plexopathies osteonecrosis malignant bone tumors and fibrous replacement of many tissues. Glenohumeral cartilage and subchondral bone are on occasion affected by these changes and may require treatment by prosthetic arthroplasty or other alternative methods.
Septic arthritis of the shoulder is uncommon but when it occurs it is often in a person debilitated from a generalized disease (Baker Oddis Medsger 1987; Burdge Reid Reeve et al. 1988) in a person on immunosuppressive medications or in a person who has an underlying shoulder disease process such as rotator cuff tearing (Armbuster Slivka Resnick et al. 1977) or rheumatoid arthritis. (Kraft Panush and Longley 1985) In this latter setting there appears to be an exacerbation of the underlying shoulder disease and in the absence of fever or an elevated white blood count diagnosis will depend on a high level of suspicion joint aspiration and bacteriological testing. Leslie et al (Leslie Harris and Driscoll 1989) reviewed 18 cases of shoulder sepsis of which 11 had Staph aureus. Some were initially confused with non-septic arthritis and treated with anti-inflammatory agents. The results of treatment were poor but somewhat better with arthrotomy than repeated aspiration.
Neoplasia present insidiously; it is often characterized by non mechanical pain. The tumor may incite a synovial response mimicking an arthritic condition. (Benjamin Hirschowitz Arden et al. 1982; Medsger Dixon Garwood 1982) The pain may be more intense than the usual arthritic pain and decidedly unresponsive to rest. Diagnosis will depend on accessing the patient's general health high quality plain x-rays and additional imaging modes including tomography computerized tomographic scanning bone scanning or magnetic resonance imaging. Identification of the primary lesion in metastatic disease is desirable but sometimes biopsy of the shoulder lesion is the most direct route to diagnosis.