Edited by Nick Hernandez, M.D., Assistant Professor, UW Orthopaedics & Hip & Knee
In this article:
- Basics of hip arthritis
- Symptoms
- Impacts on daily life
- Conditions with similar symptoms
- Causes
- Diagnosis
- Treatment
- Research
- Summary of osteoarthritis of the hip
Basics of hip arthritis
Many kinds of arthritis can affect the hip joint. The most common type of hip arthritis is osteoarthritis, which some people call "degenerative joint disease."
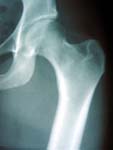
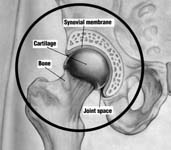
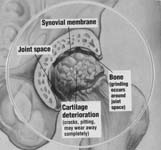
Osteoarthritis occurs when the joint surface cartilage (also called hyaline cartilage or articular cartilage) becomes worn away leaving the raw bone beneath exposed. The cartilage normally serves as a “pad” or a bearing in the joint. Under normal conditions, the cartilage bearing is slicker than a hockey puck on ice. When the bearing wears away, the result is a roughed joint surface that causes the pain and stiffness that people associate with osteoarthritis (See Figures 1-4).
Osteoarthritis of the hip is a serious condition. Osteoarthritis is the most common of the more than 100 kinds of arthritis and the hip joint is the second most commonly affected large joint in the body.
Osteoarthritis is a chronic disease that can takes months to years to appear. While it is not “curable,” it most certainly is treatable using activity modifications, medications, and/or injections. If those interventions don’t work, hip replacement surgery often will relieve the pain associated with hip arthritis.
Osteoarthritis of the hip results in pain, stiffness, and joint deformity. The symptoms of osteoarthritis can affect one’s ability to walk, work, and enjoy life.
For most patients who have mild arthritis, pain can be managed with ice, rest, activity modifications, pills, or joint injections.
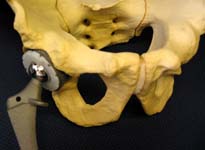
However, for patients with severe arthritis, the pain may not respond to those kinds of interventions. Patients with severe arthritis sometimes can benefit from total hip replacement surgery (See Figures 5 and 6).
Hip Arthritis Image Gallery
Click an image below to enlarge.
Symptoms of Hip Arthritis
Initial symptoms
Hip joint pain and stiffness are the main symptoms of hip arthritis. When it becomes more advanced, joint deformities and leg-length differences can result.
The typical pain from hip arthritis is located in the groin thigh or buttock. The pain is generally worse with weight bearing activities (e.g., walking, standing, or twisting).
Some patients report "start-up" pain – an especially bad discomfort upon standing after being seated for a prolonged period of time. This sometimes works itself out after a few steps.
Osteoarthritis of the hip is not an emergency. It can however result in disturbing “flare ups ” with increased pain and stiffness. Many patients who experience a sudden flare-up will go to the doctor for care. For many of these patients, this “acute” set of symptoms will result in the diagnosis of osteoarthritis.
Progression
Early in the course of arthritis, symptoms can be intermittent, perhaps related only to particular activities or sustained activity. Rest and avoiding the precipitating activity will improve the symptoms.
As arthritis worsens, symptoms can become more persistent or more severe, such that simply walking on level ground can result in pain.
When arthritis is severe, the pain with activities can linger even after the activity stops. When arthritis is severe, the hip can remain painful even after one stops walking.
As the condition worsens it often becomes less responsive to medical treatments such as pills or injections.
In many patients with advanced arthritis, particularly if those medical approaches are no longer helpful, surgery can offer relief of symptoms. Some patients with severe osteoarthritis sometimes can benefit from total hip replacement surgery.
Impacts on Daily Life
Daily activities
Osteoarthritis of the hip can affect one’s ability to walk, climb stairs, enter or exit a vehicle, sit or arise comfortably, perform housework and enjoy one’s day-to-day activities.
Even mild to moderate osteoarthritis of the hip can adversely impact athletic performance and enjoyment of sports, particularly impact sports and sports that involve running.
Energy
Many patients find that the chronic pain associated with osteoarthritis of the hip does contribute to fatigue.
Osteoarthritis of the hip does not affect metabolism but some patients attribute weight gain to the inactivity that results from the hip pain caused by osteoarthritis of the hip.
Mobility and independence
Osteoarthritis of the hip can affect one’s ability to walk, climb stairs, enter or exit a vehicle and enjoy one’s day-to-day activities. These things do affect one’s ability to remain independent particularly as the disease reaches its more severe stages.
Fertility and pregnancy
Osteoarthritis of the hip can cause sexual intercourse to be uncomfortable in some patients. However, apart from that, it will not affect a patient’s ability to get pregnant or have children. It is important to note, though, that some medications used to treat arthritis need to be used with care (or not at all) during a pregnancy. It is important to inform one’s obstetrician and family physician about all medications and nutritional supplements that one takes.
Relationships
Osteoarthritis of the hip can affect relationships and social interactions to the extent that it makes getting around more difficult. In some patients with more severe hip arthritis, sexual intercourse can be uncomfortable because of the pain associated with moving the hips that accompanies the condition.
Joint deformity
Osteoarthritis of the hip is associated with joint deformity that sometimes results in a leg-length inequality. These joint deformities, including leg-length inequality, are not readily managed by interventions other than surgery but can sometimes be corrected at the time of hip replacement for patients who elect to have that surgery. Shoe lifts can help patients before surgery who have leg-length inequalities and are sometimes used if the leg length cannot be made equal at the time of hip replacement surgery.
Conditions with similar symptoms
A number of conditions that are not actually related to the hip joint can cause hip joint pain and symptoms in the "hip" area. These include:
Spinal stenosis (arthritis of the lower back)
This condition most commonly causes pain in the buttock, low back, and back of the upper thigh (See Fig. 7). Spinal stenos is a lower-back problem, not a hip problem. Spinal stenosis causes pain in the buttock area that some identify as part of the "hip."
Greater trochanteric bursitis
This causes pain over the “point” of the hip (imagine the part of the hip that would touch the ground if one were to lie directly on one’s side (See Fig. 8). It also causes tenderness and sensitivity to pressure. Although this seems like a “hip” problem, it is a problem well away from the joint itself and is related to an inflammation in a “lubrication point” called a bursa. Greater trochanteric bersitis is not a joint problem (and only rarely is it a surgical problem).
Click an image below to enlarge.
Non-orthopedic conditions
Very occasionally, non-orthopedic conditions can cause pain in the groin that masquerades as hip joint symptoms – ovarian cysts, hernias, and other intra-pelvic conditions can sometimes cause pain that is mistaken for hip joint pain.
Other types of arthritis
Other forms of arthritis can cause similar symptoms to osteoarthritis of the hip; in particular, post-traumatic arthritis and avascular necrosis (osteonecrosis) are almost indistinguishable in many cases from osteoarthritis of the hip.
Rheumatoid arthritis
Rheumatoid arthritis, the next most common cause of arthritis, can also affect the hip. It tends to cause other joints to be involved and often causes more of an inflammatory set of symptoms (swelling and warmth as well as pain) and can, in fact, affect other organ systems as well.
The diagnosis of osteoarthritis versus rheumatoid arthritis can be made by a physician with experience in treating conditions of this type.
Causes
It is not possible to predict who will get osteoarthritis of the hip. However, there are some risk factors that may increase the likelihood that hips will become arthritic. These risk factors include:
- Genetics - Arthritis often runs in families.
- Childhood hip diseases including developmental hip dysplasia (DDH), Legg-Calve-Perthe’s Disease and slipped capital femoral epiphysis (SCFE) all can predispose an individual to premature hip arthritis.
- Acquired conditions such as avascular necrosis (osteonecrosis) can result in hip arthritis if left untreated or if treatment fails. Avascular necrosis can be caused by excessive alcohol intake, some medications (including prednisone a medical steroid), and some medical conditions that affect blood clotting.
- Variations in hip anatomy (the shape of the hip joint itself) including a condition called femoroacetabular impingement can cause the hip to become arthritic.
- Severe trauma. Fractures (broken bones) or traumatic dislocations of the ball from the hip socket can, in time, result in arthritis of the hip. Whether this really is “osteoarthritis” or should be considered a separate kind of arthritis (post-traumatic arthritis) remains an open question. Though, in the severe stages of this condition the treatments are the same.
- Obesity. Some studies have associated this condition with arthritis of the hips. Though interestingly, obesity is more strongly linked to arthritis of the knees than to arthritis of the hips.
Diagnosis
To diagnose osteoarthritis of the hip, a physician will take a thorough history and perform a thorough physical examination first. Following this, simple x-rays taken with the patient standing are an effective way to diagnose this condition.
Diagnostic tests
The simplest test to diagnose osteoarthritis of the hip is the x-ray. Taken with the patient standing up plain x-rays can diagnose the condition with great accuracy.
Very mild arthritis can be seen on a bone scan or an MRI even before it is visible on plain x-rays, but in reality, these tests are seldom helpful clinically for this purpose.
Effects
The diagnostic tests for osteoarthritis of the hip, including x-rays and MRIs, are generally not painful and they are well-tolerated by most patients.
Treatment
Simple steps that can be taken which don’t have much risk include avoidance of the activities that cause symptoms (activity modification) and weight loss (if appropriate). Some patients find nutritional supplements, such as glucosamine and chondroitin, to be helpful. However, the data on these products is somewhat inconsistent. They don’t help everyone.
Should those interventions not be satisfying, in consultation with one’s physician, the next steps might include over-the-counter pain remedies such as acetaminophen (Tylenol) and over-the-counter anti-inflammatories such as ibuprofen (Advil Motrin) or naproxen (Naprosyn), among others. However, these pills are not for everyone and if one hasn’t used them before one should consider consulting one’s family physician first. Sometimes prescription-strength, non-steroidal, anti-inflammatory drugs (NSAIDs) can be prescribed; but again, this must be done in consultation with a physician and these drugs do have risks and side effects associated with them.
In general, narcotic pills (“painkillers” like Tylenol #3 Vicoden Percocet oxycodone) and narcotic pain patches (fentanyl Duragesic) should be avoided for most patients with osteoarthritis of the hip.
Joint injections including intra-articular corticosteroid injections can be helpful for some patients. However, joint injections generally appear to be less useful for hip arthritis than they are for arthritis in other joints, in part because of the difficulty of injecting the hip joint accurately.
Patients with severe arthritis who have tried the above remedies sometimes can benefit from total hip replacement surgery.
Self-management
Keeping one’s body weight appropriate and choosing activities that don’t reproduce the arthritic pain are two things patients with osteoarthritis of the hip can do to help decrease their arthritic symptoms.
Health care team
Several kinds of health care providers participate in the management of osteoarthritis of the hip including:
- Family physicians and internists
- Rheumatologists
- Physical Medicine and Rehabilitation Specialists (Physiatrists)
- Orthopedic Surgeons
Finding a doctor
Both rheumatologists and orthopedic surgeons are “specialists” in arthritis care.
If surgery is being considered to manage osteoarthritis of the hip, visiting with a fellowship-trained, high-volume hip replacement surgeon would be a reasonable step to consider.
Managing arthritis pain and fatigue
Several approaches can be used to manage the pain associated with osteoarthritis of the hip including:
- Activity modification appropriate kinds of exercise and weight loss when necessary may alleviate some hip arthritis symptoms
- Nutritional supplementation (glucosamine and chondroitin) are helpful to some patients, although the literature on these supplements is not consistently in favor of their use
- Non-narcotic pain tablets (acetaminophen/Tylenol), or over-the-counter non-steroidal anti-inflammatory drugs, if medically appropriate, sometimes are helpful
- Prescription strength, non-steroidal, anti-inflammatory drugs (NSAID) are useful for some patients, though, in general, long-term use of these drugs is discouraged
- Arthritis unloader braces or hip sleeves are helpful for some patterns of arthritis
- Joint injections (corticosteroid or “cortisone” injections) might help
- Total hip replacement surgery may be used if non-operative interventions don’t suffice.
Diet
Keeping one’s weight proportional to one’s height can decrease the likelihood of developing osteoarthritis of the hip and can decrease the symptoms of the condition once it has set in.
Exercise and therapy
There is some limited evidence that appropriately-designed exercise programs can decrease the pain of hip arthritis, in particular, earlier stages of the condition. In general, staying fit and height-weight proportional also are helpful.
Medications
- Nutritional supplementation (glucosamine and chondroitin) are helpful to some patients although the literature on these supplements is not consistently in favor of their use.
- Non-narcotic pain tablets (acetaminophen/Tylenol) or over-the-counter, non-steroidal, anti-inflammatory drugs, if medically appropriate, sometimes are helpful.
- Prescription strength, non-steroidal, anti-inflammatory drugs (NSAID) are useful for some patients, though, in general, long-term use of these drugs is discouraged.
- Joint injections (corticosteroid or “cortisone” injections) might help.
- Narcotic painkillers, in general, whether in pill form (oxycodone Tylenol #3 Vicoden Percocet Lortab etc.) or patch form (Duragesic fentanyle etc.), should be avoided for the treatment of osteoarthritis of the hip.
Surgery
Hip replacement is a surgical procedure that decreases pain and improves the quality of life in many patients with severe arthritis of the hips.
Typically, patients undergo this surgery after non-operative treatments (such as activity modification anti-inflammatory medications or hip joint injections) have failed to provide relief of arthritic symptoms.
Surgeons have performed hip replacements for over four decades ,generally with excellent results. Most reports have ten-year success rates in excess of 90 percent.
Learn more about total hip replacement surgery.
Joint aspiration
Joint injections can be effective at relieving the symptoms associated with osteoarthritis of the hip. Broadly speaking, there are two kinds of injections:
- Corticosteroid injections ("cortisone shots") - These injections have been used to relieve arthritis symptoms--including pain swelling and inflammation--for over 50 years. Despite this, there have been surprisingly few well-designed scientific studies to determine which patients might benefit from this treatment or how long the relief might last.
Just the same, cortisone shots are commonly used--and often are successful--in helping to relieve arthritis symptoms temporarily. Some patients are able to use them to get enough pain relief to hold off joint replacement surgery for months or even years. Cortisone shots are a treatment for pain; they do not alter the course of arthritis and they do not cure the condition. In general, they are more commonly used for arthritis of other joints than they are for arthritis of the hip joint. - "Viscosupplement" injections - These are any of several compounds that are made up of hyaluronic acid which is a component of normal joint fluid. Some of the common ones include Synvisc Hyalgan Supartz and Orthovisc. They are given as a series of injections usually weekly for 3-5 weeks. There is some disagreement as to how and whether they work. Read more details on JBJS Article - Corticosteroids VS. Hylan GF20 in pdf format (0.13MB). They are FDA-approved for managing the pain associated with arthritis of the knee but they are not, as of December 2007, FDA-approved for use in the hip joint.
Hip arthritis patients who have perceptible leg-length inequalities can be managed with a shoe lift either inside the shoe (typically if the difference is <1/4”) or built onto the outside of the shoe (if the difference is larger).
Alternative remedies and treatments
Nutritional supplementation (glucosamine and chondroitin are the most common forms of this) is helpful to some patients though the science on this is not entirely supportive of their effectiveness.
There are some studies to suggest that acupuncture can decrease the pain associated with osteoarthritis of the hip.
Although there is little “hard science” on this point, most hip surgeons and rheumatologists (doctors who treat arthritic conditions non-operatively) believe that patients with osteoarthritis of the hip should consider avoiding impact sports such as running in order to avoid increasing the rate at which the disease progresses.
It is important that patients with osteoarthritis of the hip avoid decreasing their activity level and it is important that they remain fit. However this often does require some modification of exercise programs – running and walking programs are usually poorly tolerated by (and not recommended for) patients with osteoarthritis of the hip. Stationary bike, swimming and water aerobics usually are well-tolerated and they are recommended.
Work
Looking for a "light duty" alternative to heavy manual labor is one good approach for coping with osteoarthritis of the hip.
Many patients who work at desks find that prolonged sitting in one position is associated with stiffness and pain upon first arising so periodically standing stretching or moving the hip through an arc of motion can be helpful at minimizing this “start-up” pain.
Adaptive aids
For some patients, particularly those who cannot tolerate surgical interventions for medical or other personal reasons, use of a cane crutches or a walker can be of use.
Additional Resources
For more information about arthritis contact the Arthritis Foundation (www.arthritis.org).
For more information about orthopedic surgery contact the American Academy of Orthopedic Surgeons (www.aaos.org).
Research on osteoarthritis of the hip
Condition research
Medical researchers continue to look into the causes and best treatments for symptoms of osteoarthritis of the hip, which is very common and sometimes disabling.
Pharmaceutical research
There is considerable research being done into the medical management of osteoarthritis which is increasing awareness of the complications and problems associated with use of non-steroidal anti-inflammatory drugs (NSAIDs), including their effects on the kidneys, the stomach, and the heart.
Surgical research
There is considerable research being done studying the surgical approaches for this condition, including newer approaches for total hip replacements and newer implants.
Other surgical interventions, including osteotomy (cutting and re-orienting the bones around the hip) and arthroscopy (using a surgical camera and small motorized shavers to "clean up" the raw bone ends), also are topics of surgical research that may someday be relevant to patients with hip arthritis.
Summary of hip arthritis
- Osteoarthritis of the hip is common and can result in severe hip joint pain and disability. as a result of this condition, several hundred thousand people each year in the U.S. undergo total hip replacement.
- Most people with osteoarthritis of the hip can be managed without surgery.
- The cause of osteoarthritis of the hip is not known but some risk factors include obesity, severe hip trauma, and acquired conditions in adulthood, such as osteonecrosis (avascular necrosis) and genetics.
- There are many other kinds of arthritis that can affect the hip. It is important to make sure that the correct diagnosis is made as some of these other conditions are treated very differently.
- The diagnosis of osteoarthritis of the hip is usually very straightforward and is made in almost all cases by a physician taking a thorough history, performing a physical examination, and getting x-rays with the patient standing up.
- Patients usually seek care for the typical symptoms of hip arthritis, including pain located in the groin thigh or buttock. The pain associated with osteoarthritis of the hip is generally worse with weight bearing (walking standing) or twisting. Stiffness and leg-length inequality are other symptoms.
Facts and myths
Following are several misconceptions about osteoarthritis of the hip.
MYTH: Osteoarthritis of the hip is usually the result of “overuse.”
FACT: Osteoarthritis of the hip is NOT usually the result of "overuse." There have been studies of long-distance runners that show that they are not more likely to get arthritis than more sedentary individuals.
MYTH: Osteoarthritis of the hip is a “normal result of aging.”
FACT: Many older people – in fact most – DO NOT develop arthritis of the hip and many younger people do experience osteoarthritis.
MYTH: Osteoarthritis of the hip is just “aches and pains.”
FACT: Osteoarthris of the hip is NOT just "aches and pains." Osteoarthritis of the hip is a condition whose biology, x-ray appearance and clinical symptoms are defined.
MYTH: Not much can be done for osteoarthritis of the hip.
FACT: While it is not “curable”, it most certainly is treatable using activity modifications, medications, injections and if those interventions, don’t work hip replacement surgery often will relieve the pain associated with hip arthritis. In fact, there are exercise programs that can alleviate the pain in mild arthritis, a variety of medications can be helpful for moderate arthritis, and severe arthritis of the hip is very commonly successfully treated with hip replacement surgery.