Overview
Follow Dr. Matsen's Shoulder Arthritis blog.
Basics of fibromyalgia
"Fibromyalgia" is a name used to describe generalized muscular pain and fatigue.
Fibromyalgia is a set of signs and symptoms that occur together (A sign is what the physician finds on examination; a symptom is what a person reports to the doctor). Although fibromyalgia may feel like a joint disease, it is not a true form of arthritis and does not cause deformities of the joints.
Prognosis
Fibromyalgia is not damaging to the body, but it may be a chronic condition. A carefully planned treatment program is essential. With proper management and a positive attitude, most people with fibromyalgia improve and are able to deal with their condition.
Incidence
Fibromyalgia is a common condition in the US affecting 3.4% of women and 0.5% of men.
Symptoms
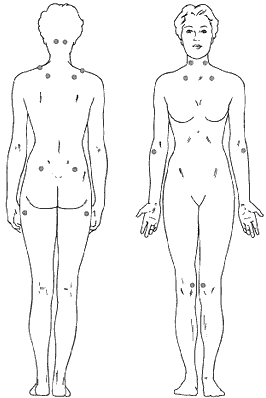
possible locations
of tender points
In fibromyalgia, generalized widespread muscular pain and tender points (see figure 1) may be present. Pain is generally felt all over, although it may start in one region, such as the neck and shoulders and seems to spread over a period of time. Fibromyalgia pain has been described in a variety of ways including: burning, radiating, gnawing, sore, stiff and aching. It often varies according to time of the day, activity level, weather, sleep patterns and stress levels. Most people with fibromyalgia say that some degree of pain is always present. They sense that the pain is mainly in their muscles and often note that fibromyalgia feels like a persistent flu.
About 90 percent of people with fibromyalgia describe moderate or severe fatigue with lack of energy, decreased exercise endurance or the kind of exhaustion felt with the flu or with lack of sleep. Often the fatigue is more of a problem and more troubling than the pain. Generally, people with fibromyalgia wake up feeling tired, even after sleeping throughout the night. They may be aware that their sleep has become lighter and that they wake up during the night. Scientific studies have demonstrated that most people with fibromyalgia have an abnormal sleep pattern, especially an interruption in their deep sleep.
The fatigue in fibromyalgia is similar to that in another condition called chronic fatigue syndrome (CFS). Some people with fibromyalgia have symptoms of CFS and vice versa. For example, many people with CFS have the tender points and symptoms considered to be diagnostic of fibromyalgia.
Changes in mood and thinking are common in fibromyalgia. Many individuals feel "blue" or "down, although only about 25 percent are truly depressed at the time of diagnosis, many people with fibromyalgia have a personal history of depression or anxiety at some time in their life. Mood disorders share many similar symptoms with fibromyalgia and vice versa.
There is evidence that some people with fibromyalgia have a history of abuse or neglect during their life as well. It is not clear yet what role these issues might play in the development and continuation of fibromyalgia, but these are important things to discuss with your health care provider since addressing such issues may help reduce the symptoms of fibromyalgia and help the person affected cope with the illness.
As with other chronic illnesses, people with fibromyalgia may report difficulty concentrating or performing simple mental tasks. There is no evidence that these problems become more serious. Similar problems have been noted in many people with sleep disturbances of all kinds or with mood changes.
People with fibromyalgia may have feelings of numbness and tingling in their hands, arms, feet, legs or sometimes in their face. These feelings can suggest other disorders, such as carpal tunnel syndrome, neuritis or even multiple sclerosis. Therefore, people with fibromyalgia often undergo numerous tests for such conditions, only to find that the test results are normal.
Headaches especially muscular (tension) and migraine headaches are common in fibromyalgia. Abdominal pain, bloating and alternating constipation and diarrhea are also common. This may resemble irritable bowel syndrome or "spastic colon." Similar bladder spasms and irritability may cause urinary urgency or frequency.
Causes
Most people with fibromyalgia do not remember any specific event that lead to their symptoms. Some people feel that fibromyalgia was triggered by stresses, such as an illness, emotional trauma or hormonal changes. These stresses may precipitate the generalized pain, fatigue and sleep and mood problems that characterize fibromyalgia.
Physical or emotional trauma could precipitate fibromyalgia in a number of ways. For example, a physical trauma such as having an infection or flu could lead to certain hormonal or chemical changes that promote pain and worsen sleep. In addition, people with fibromyalgia may become inactive, depressed and anxious about their health, further aggravating the disorder. Smoking and inappropriate exercise or poor posture may aggravate fibromyalgia. The tender points mentioned above have been shown to indicate that a person is under stress. People with fibromyalgia may internalize their stress, i.e. keep it inside and then it is expressed as muscle tension and pain.
Diagnosis
The diagnosis is usually based on talking to your health care provider and having an examination done.
There are 18 points (9 on each side of the body) that are tender to touch. Most of these are around the neck and shoulders. Someone who has seen people with fibromyalgia usually has no problem finding these tender points. The rest of the examination is usually normal, unless other medical conditions are also present unrelated to fibromyalgia.
Diagnostic tests
Your health care provider will usually check a series of blood tests to look for other possible conditions that might mimic fibomyalgia. Low thyroid hormone (hypothyroidism) typically causes fatigue, cold intolerance, muscle aches and pain and weight gain. Anemia also may lead to fatigue and exercise intolerance. People with abnormally high or low levels of calcium in their blood may also have similar symptoms. Several muscle disorders may mimic fibromyalgia and can be checked with a blood test called the CPK. Certain inflammatory disorders may also appear to be fibromyalgia and can be detected by examination and by checking a blood test for inflammation called the ESR. As mentioned above, depression can mimic symptoms of fibromyalgia and knowing whether this is present or not may have profound impact on treatment. Therefore, it is important to know if depression is present. This can usually be detected by a few simple questions.
Treatment
As with most chronic illnesses, the treatment should be tailored to meet your individual needs.
Some people with fibromyalgia have mild symptoms and need very little treatment once they understand what fibromyalgia is and what worsens their condition. Most people do benefit from a comprehensive care program. Some treatment strategies include:
- Education about the illness and reassurance that it is not usually disabling
- Progressive exercise programs that involve stretching and cardiovascular fitness
- Relaxation techniques and other measures to help you relax tense muscles and release stress
- Non-narcotic medications that diminish pain and improve sleep
- Treatment of depression or other mood disorders, if present
- Counseling, if needed
- Continued involvement in the enjoyable and productive aspects of life
Exercise and therapy
Two principles of treating fibromyalgia are to increase cardiovascular (aerobic) fitness and to stretch and mobilize tight sore muscles. You may be reluctant to exercise if you are already in pain and feel tired. Low or non-impact aerobic exercises such as brisk walking, biking, swimming or water aerobics are generally the best way to start such a program. Exercise on a regular basis, such as every other day and gradually increase to reach a better level of fitness. Some people can greatly reduce their symptoms with exercise.
Gently stretch your muscles and move your joints through an adequate range of motion daily and before and after aerobic exercise. Physical therapy may be helpful and could include techniques such as: heat, ice, massage, whirlpool, ultrasound and electrical stimulation to help control pain. Physical therapists may also be consulted to design a specific exercise program to improve posture flexibility and fitness.
Medications
The anti-inflammatory medications used to treat arthritis and many rheumatic conditions do not have a major effect in fibromyalgia. However, modest doses of aspirin, ibuprofen or acetaminophen may help to provide some pain relief and lessen stiffness. Narcotic pain relievers, tranquilizers and cortisone derivatives have been shown to be ineffective and should be avoided because of their potential side effects.
Medications that promote deeper sleep and also relax muscles help many people with fibromyalgia. These include amitriptyline (Elavil), doxepin (Sinequan), cyclobenzaprine (Flexeril) and related medications. Although these medications are also used to treat depression, in people with fibromyalgia they are generally used in very low doses and only at bedtime. Thus, they are not specifically used as antidepressants or tranquilizers in the treatment of fibromyalgia but may relieve pain and improve sleep.
Although many people sleep better and have less discomfort when they take these medications, the improvement varies greatly from person to person. In addition, the medications may have side effects such as daytime drowsiness, constipation, dry mouth and increased appetite. These side effects are rarely severe but can be disturbing and may limit the use of these drugs. Therefore, a number of different medicines may need to be tried and doses adjusted in consultation with a doctor.
Strategies for coping
Often people with fibromyalgia have undergone many tests and have seen many different specialists while in search of an answer. This leads to fear and frustration which may increase the pain.
People with fibromyalgia are often told that since they look well and their tests are normal, they are not suffering from a real disorder. Their family and friends as well as physicians may doubt the reality of their complaints, increasing their feelings of isolation, guilt and anger.
You and your family should understand that fibromyalgia is definitely associated with chronic pain and fatigue and must be dealt with as with any chronic illness. Yet fibromyalgia is not life-threatening and causes no deformity. Although symptoms may vary, the overall condition rarely worsens over time.
Often just knowing fibromyalgia is not a progressive crippling disease allows people to stop additional expensive testing and develop a more positive attitude toward their condition. Relaxation techniques such as meditation, visual imagery, progressive muscle relaxation, yoga or biofeedback may also be helpful. You should examine your own sleep patterns and avoid aggravating factors, such as excess caffeine and alcohol. If you feel depressed or very anxious, it is important to get help from a mental health professional. The more you learn about your condition and the more you take an active role in finding the best means to lessen your symptoms, the better the outcome.
Condition research
Much research is now being done to try to understand both the psychological aspects and biological aspects of fibromyalgia with the hope that a holistic understanding will lead to a holistic treatment approach. Certain brain chemicals and pain receptors have been found to be altered in people with fibromyalgia and chronic pain in general. Research is being directed toward trying to modify these abnormalities to relieve the pain and fatigue.
Credits
Some of this material may also be available in an Arthritis Foundation brochure.
Adapted from the pamphlet originally prepared for the Arthritis Foundation by Don L. Goldenberg, M.D. This material is protected by copyright.