Basics of hallux valgus (bunions)
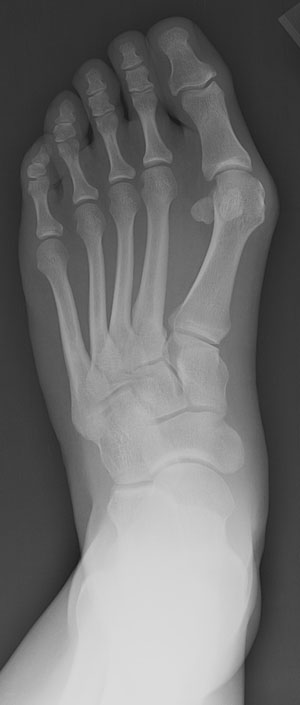
Hallux valgus is a condition in which the big toe migrates laterally toward the second toe. This results in a bump on the inner side of the foot know as a bunion. It is related to a combination of genetic factors, activities and inheritance. Some patients who have this condition do not have symptoms. Sometimes symptoms can be relieved just by modifying the shoe to have enough room in the forefoot to accommodate the changed shape.
Diagnostic tests
Examination by a qualified physician is important if the problem hurts or is worsening. Diagnostic tests may include:
- Physical examination to determine if there are tendons such as the Achilles that are too tight or if there is instability in a joint or joints that contribute to the problem.
- X-ray of two views of the foot while you are standing on it.
- Specialty studies may be involved if there are unique aspects to the problem.
Not all surgical cases are the same, this is only an example to be used for patient education.
Surgery
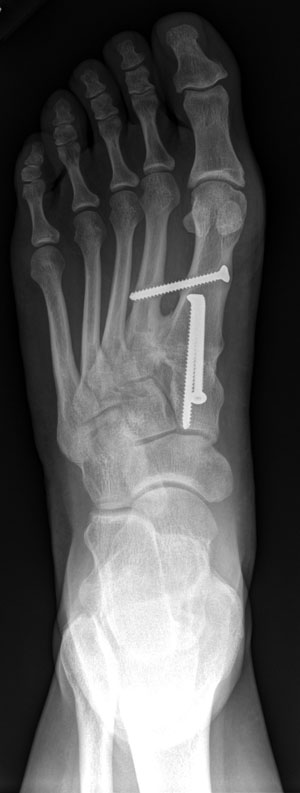
The goal of surgery is to remove any predisposing conditions, such as an excessively tight Achilles tendon, straighten the metatarsal and straighten the toe.
There are a variety of surgical techniques that accomplish these goals. The surgical technique chosen should be individualized to the specific type of deformity. Many of the procedures can be done as an outpatient. The more involved procedures may require a hospital stay of one to three nights.
Some of the surgical procedures will require that either the bone is cut and returned to a normal position or that a joint undergoes a procedure known as arthrodesis. This means that a small joint is bridged by bone in order to maintain the position of the bones in relation to one another.
Often there are other associated deformities with hallux valgus such as toes that are too curled or overloading of the metatarsal head sometimes known as the ball of the foot. These issues can be addressed simultaneously.
There are over 150 different surgical procedures described for correction of these forefoot problems. It's best to meet with a qualified physician to discuss options for your foot.
UW team for surgery
The UW Department of Orthopaedics and Sports Medicine is composed of many different health care experts who function as a team to make surgery safe and effective. This team includes senior and more junior physicians, physician assistants, nurses, physical therapists and support personnel. Office visits are scheduled through the office staff. Surgery is scheduled through a patient care coordinator and various aspects of your care are provided by other personnel. Surgery is under the care of surgeons.
Hospital stay and discharge
Surgery is usually scheduled as an outpatient or a same-day admission-type surgery. This means that you will come to the hospital on your day of surgery and either go home the same day or be admitted to the hospital. Depending on the type of surgery done, the hospital stay may be one night or two. If extensive reconstruction is done in other parts of the foot, a third night may be necessary. In general, you will be protected in some type of boot or cast and using crutches for about six weeks.
Pain management
For the first 24 to 48 hours, you will receive parenteral pain medicine. This means medicine injected with a syringe. After that, oral narcotic medication will be provided. Please follow the recommendations on the pain prescription.
Follow-up
You will return to the outpatient center two weeks after the surgery for removal of your sutures and a wound check. During that time, you will need to keep the dressing dry and your foot elevated. Four weeks after this first outpatient visit, a second outpatient visit will be scheduled at which time x-rays will be performed. Based on the x-rays, the activity will be determined.
Wound Care
The bandage will have to be kept clean and dry. You may shower with a plastic bag securely draped over the dressing. It is recommended that you obtain a plastic shower chair to avoid falling in the shower.
Rehabilitation
Rehabilitation with a physical therapist will begin immediately after surgery with crutch training and extend to full recovery. You will use crutches for a period of time specified by your physician. A brace or cast will be worn.
You will also be asked to do straight leg raising and quadriceps sitting exercises. For quadriceps sitting, you lie on your back with your knees straight, legs flat and arms by your sides. You tighten the muscles on the top and the front of the thigh called the quadriceps and at the same time push the back of the knee down into the bed and raise only the heel. Hold for five seconds and relax for five seconds. Repeat this exercise 10 times on a firm surface, once per hour during the first postoperative day and at least four times a day thereafter. Straight leg raising involves lying on your back with arms and legs straight. With one knee bent and the foot flat, slowly raise the operative side about six inches off the floor keeping the leg as straight as possible. Hold for a five-second count then lower the leg. Repeat this exercise 10 times for each leg.